Patterns and Inhibition of Cell Death During Static Cold Storage of Human Kidneys
1Surgery, Yale School of Medicine, New Haven, CT, 2Biomedical Engineering, Yale University, New Haven, CT, 3Surgery, University of Cambridge, Cambridge, United Kingdom, 4Biochemistry and Medicine, Wilf Family Cardiovascular Research Institute, Albert Einstein College of Medicine, Bronx, NY, 5Surgery, Albert Einstein College of Medicine, Bronx, NY, 6Immunobiology, Yale University, New Haven, CT, 7Surgery and Biomedical Engineering, Yale School of Medicine, New Haven, CT
Meeting: 2021 American Transplant Congress
Abstract number: 530
Keywords: Image analysis, Kidney, Preservation, Renal ischemia
Topic: Basic Science » Cellular Therapies, Tissue Engineering/Regenerative Medicine
Session Information
Session Name: Cellular Therapies, Tissue Engineering/Regenerative Medicine
Session Type: Poster Abstract
Session Date & Time: None. Available on demand.
Location: Virtual
*Purpose: As the donor population continues to age and accumulate co-morbidities, more marginal kidneys are being retrieved for transplantation. However, estimates suggest that more than 40% of kidneys from extended criteria donors are discarded annually. Many of these kidneys are not considered for transplantation because we do not currently understand why these organs fail nor do we have appropriate strategies to preserve them. By studying human organs that were deemed unsuitable for transplantation, we can begin to define new modes of failure in particularly marginal organs.
*Methods: To better appreciate how kidneys respond to cold ischemia, we biopsied a series of nine kidneys at times from 12 to 72 hours of cold storage.
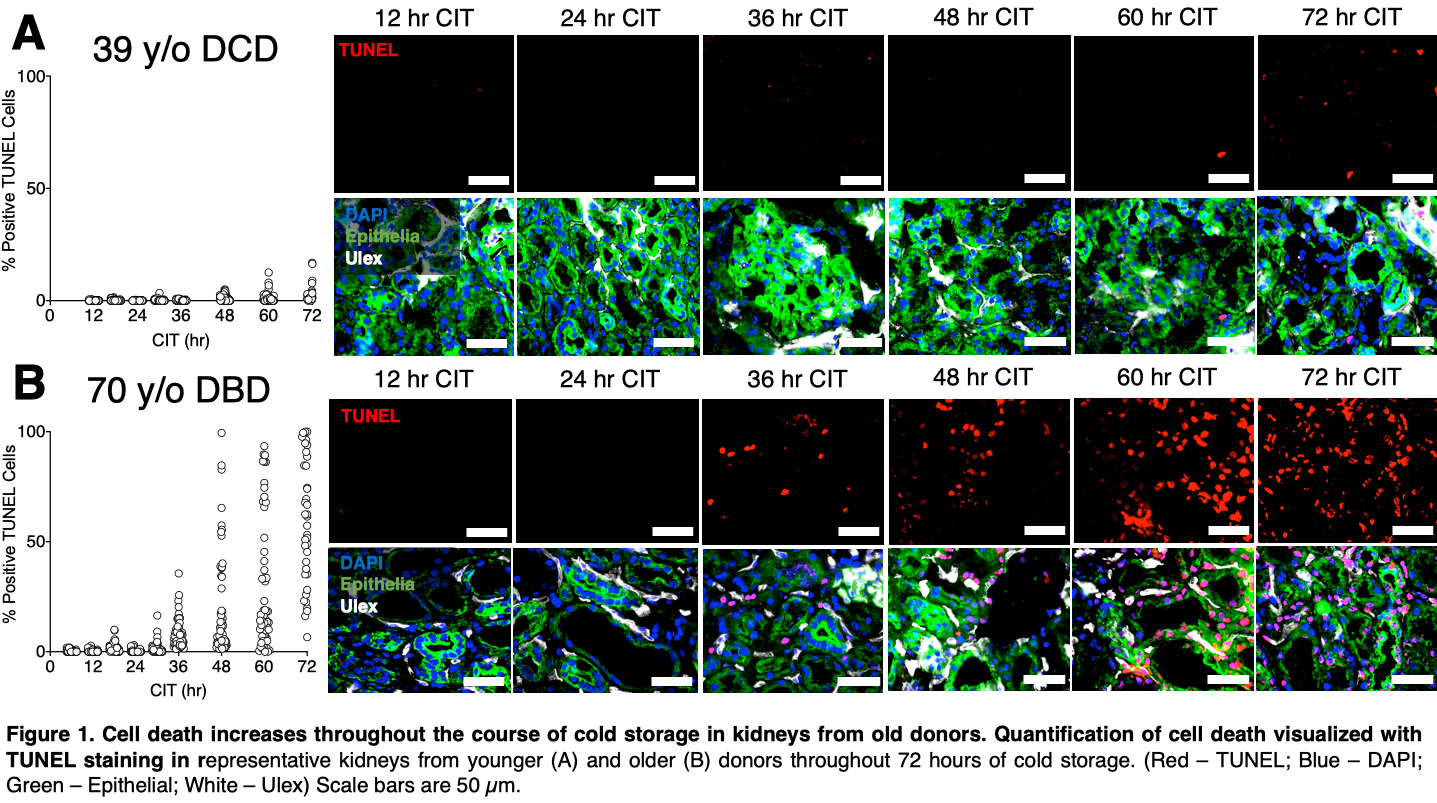
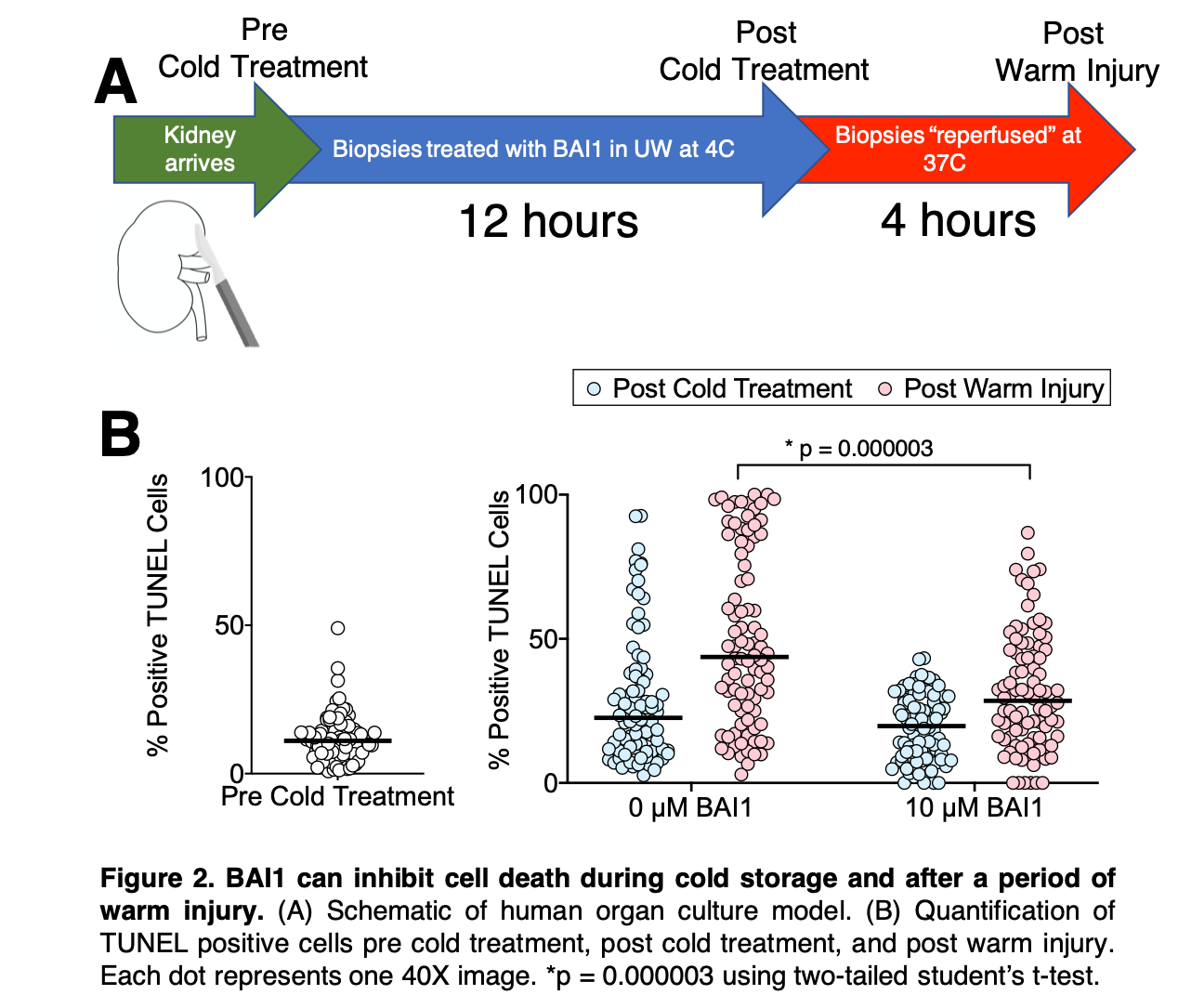
*Results: We found that older donors (70-74 y/o) had significantly more cell death visualized via TUNEL staining (Figure 1B) than younger donors (39-52 y/o) in this series (Figure 1A). Pervasive cell death throughout a biopsy became apparent in older donors between 30-36 hours of cold storage (Figure 1B). Preliminary data suggest that tubular epithelial cells are the predominate cell type positive for TUNEL staining as cold time increases. Additionally, Bax inhibitor BAI1 can significantly decrease cell death in models of human organ culture (Figure 2A), inhibiting cell death both during cold storage and after a period of warm injury.
*Conclusions: These data suggest that cell death throughout the course of cold storage can be reduced by pharmacological intervention in marginal organs and thus may improve clinical outcomes.
To cite this abstract in AMA style:
DiRito JR, Chickering G, Langford JT, Stern D, Hosgood S, Nicholson ML, Gavathiotis E, Kitsis RN, Saltzman M, Pober JS, Tietjen GT. Patterns and Inhibition of Cell Death During Static Cold Storage of Human Kidneys [abstract]. Am J Transplant. 2021; 21 (suppl 3). https://atcmeetingabstracts.com/abstract/patterns-and-inhibition-of-cell-death-during-static-cold-storage-of-human-kidneys/. Accessed May 21, 2026.« Back to 2021 American Transplant Congress