Part II: Rates and Determinants of Progression for De Novo Donor-Specific Antibody Mediated Kidney Allograft Injury
1Medicine, University of Manitoba, Winnipeg, MB, Canada
2Immunogenetics, Diagnostic Services of Manitoba, Winnipeg, MB, Canada
3Pathology, University of Manitoba, Winnipeg, MB, Canada
4Pediatric and Child Health, University of Manitoba, Winnipeg, MB, Canada
5Immunology, University of Manitoba, Winnipeg, MB, Canada.
Meeting: 2015 American Transplant Congress
Abstract number: 93
Keywords: Alloantibodies, Graft function, Graft survival, HLA antibodies
Session Information
Session Name: Concurrent Session: Kidney Antibody Mediated Rejection II
Session Type: Concurrent Session
Date: Sunday, May 3, 2015
Session Time: 4:00pm-5:30pm
 Presentation Time: 4:36pm-4:48pm
Presentation Time: 4:36pm-4:48pm
Location: Terrace I-III
The development of de novo donor-specific antibody (dnDSA) is an independent predictor of allograft loss in renal transplantation. Rates and determinants of clinical pathologic progression for recipients who develop dnDSA, especially subclinical dnDSA, are required to evaluate the effectiveness of current or novel therapies. A consecutive cohort of 560 renal transplant recipients (n=63 with dnDSA) was studied using clinical, serologic, and pathologic data. Recipients that developed dnDSA had a 3-fold increase in the rate of eGFR decline (0.36 vs. 1.07 ml/min/year, p<0.0001). Graft dysfunction at dnDSA onset was associated with a step-wise decline in eGFR of 16.5±3.0 ml/min (p<0.0001) after which subclinical and clinical dnDSA had similar rates of eGFR decline (1.32 vs 0.96 ml/min/year, p=0.446).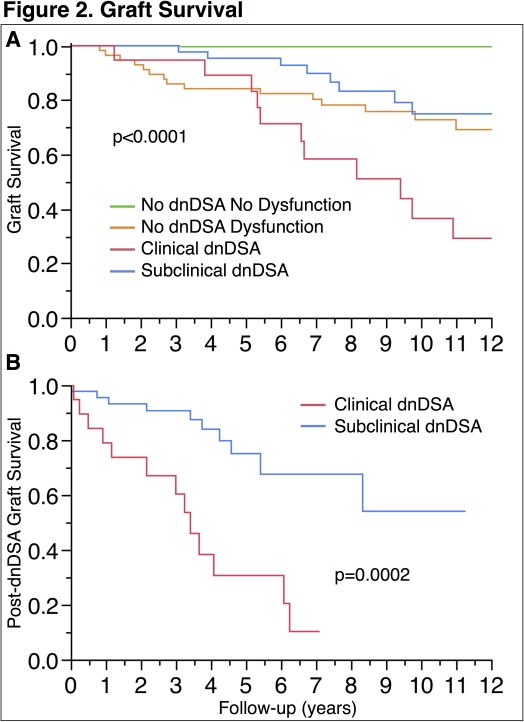 Histologic analysis of 1,088 biopsies pre and post-dnDSA development found that dnDSA independently predicted chronic glomerulopathy, but not interstitial fibrosis and tubular atrophy (IFTA), or chronic vasculopathy. Non-adherence, early cellular rejection, and time were independent predictors of IFTA. Predictors of post-dnDSA graft survival available at dnDSA detection were clinical dysfunction, dnDSA mean fluorescence intensity sum score, tubulointerstitial inflammation, and chronic glomerulopathy. Understanding the risk factors of eGFR decline and post-dnDSA detection graft loss could help design and select recipients for therapeutic trials.
Histologic analysis of 1,088 biopsies pre and post-dnDSA development found that dnDSA independently predicted chronic glomerulopathy, but not interstitial fibrosis and tubular atrophy (IFTA), or chronic vasculopathy. Non-adherence, early cellular rejection, and time were independent predictors of IFTA. Predictors of post-dnDSA graft survival available at dnDSA detection were clinical dysfunction, dnDSA mean fluorescence intensity sum score, tubulointerstitial inflammation, and chronic glomerulopathy. Understanding the risk factors of eGFR decline and post-dnDSA detection graft loss could help design and select recipients for therapeutic trials.
To cite this abstract in AMA style:
Wiebe C, Gibson I, Pochinco D, Birk P, Blydt-Hansen T, Ho J, Karpinski M, Goldberg A, Storsley L, Rush D, Nickerson P. Part II: Rates and Determinants of Progression for De Novo Donor-Specific Antibody Mediated Kidney Allograft Injury [abstract]. Am J Transplant. 2015; 15 (suppl 3). https://atcmeetingabstracts.com/abstract/part-ii-rates-and-determinants-of-progression-for-de-novo-donor-specific-antibody-mediated-kidney-allograft-injury/. Accessed May 15, 2026.« Back to 2015 American Transplant Congress
