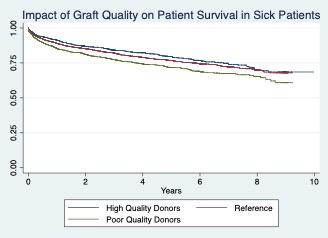
Impact of Graft Quality on Patient Survival in Sick Patients
1School of Medicine, Baylor College of Medicine, Houston, TX, 2Michael E DeBakey Department of Surgery, Division of Abdominal Transplant, Houston, TX
Meeting: 2021 American Transplant Congress
Abstract number: 186
Keywords: Graft survival, Liver, Liver transplantation, Survival
Topic: Clinical Science » Liver » Liver: MELD, Allocation and Donor Issues (DCD/ECD)
Session Information
Session Name: MELD, Allocation and Donor Issues
Session Type: Rapid Fire Oral Abstract
Date: Sunday, June 6, 2021
Session Time: 6:00pm-7:00pm
 Presentation Time: 6:25pm-6:30pm
Presentation Time: 6:25pm-6:30pm
Location: Virtual
*Purpose: It is widely accepted in the literature that patients who have a Model for End Stage Liver Disease (MELD) Score greater than 30 incur an increased survival benefit from transplantation, regardless of allograft quality, compared to patients remaining on the waitlist. While immediate transplantation with any available organ is preferential from the patient perspective, it is also important to consider allograft allocation from a societal perspective—in which case population level survival should be maximized.
*Methods: Using the Organ Procurement and Transplantation Network database, we retrospectively analyzed one-year patient survival in 7910 patients with MELD scores greater than 35. The impact of low- and high-quality allografts—quality determined by the donor risk index—was measured by adjusting for recipient risk factors in a multivariate analysis. The impact of graft quality on length of post-transplant hospital stay and graft survival were computed as well.
*Results: High quality organs were associated with 60% increased patient survival (odds ratio [OR] 0.752, p=0.006) at 1 year post-transplant compared to low quality organs (OR 1.352, p=0.001) in patients with high MELD scores. Low quality organs were also associated with increased post-transplant hospital stays and decreased graft survival.
*Conclusions: Although high risk patients experience significant survival benefit even with low quality organs, our analysis shows that selecting for high quality organs in this population is associated with better transplantation outcomes overall. Thus, there may be room for improvement in our current allocation system.
To cite this abstract in AMA style:
Handing G, Keeling S, Christmann C, Galvan N, O’Mahony C, Goss J, Cotton R, Rana A. Impact of Graft Quality on Patient Survival in Sick Patients [abstract]. Am J Transplant. 2021; 21 (suppl 3). https://atcmeetingabstracts.com/abstract/impact-of-graft-quality-on-patient-survival-in-sick-patients/. Accessed May 20, 2026.« Back to 2021 American Transplant Congress