The Impact of HLA-DQ Molecular Mismatches on De Novo Occurrence of Donor-Specific Anti-HLA Antibodies after Kidney Transplantation: An Observational Cohort Study
1Microbiology, Immunology and Transplantation, KU Leuven, Leuven, Belgium, 2HILA, Red Cross-Flanders, Mechelen, Belgium
Meeting: 2020 American Transplant Congress
Abstract number: 104
Keywords: Alloantibodies, Histocompatibility antigens, HLA matching, Immunogenicity
Session Information
Session Name: Histocompatibility and Immunogenetics
Session Type: Oral Abstract Session
Date: Saturday, May 30, 2020
Session Time: 3:15pm-4:45pm
 Presentation Time: 3:27pm-3:39pm
Presentation Time: 3:27pm-3:39pm
Location: Virtual
*Purpose: Evaluating HLA molecular mismatches (MM) instead of antigen mismatches might be a better tool to assess donor-recipient HLA incompatibility and provide a better risk assessment for primary immune response. We aimed to evaluate the impact of HLA MM on de novo DSA (dnDSA) formation in a large cohort of donor-recipient pairs with full HLA genotyping data.
*Methods: The study included all consecutive adult kidney recipients transplanted at a single center between 2004 and 2013. 926 transplant pairs were retrospectively HLA genotyped at high-resolution level for HLA -A,-B,-C,-DRB1345,-DQA1,-DQB1,-DPA1, and -DPB1. HLAMatchmaker was used to count HLA eplet mismatches.
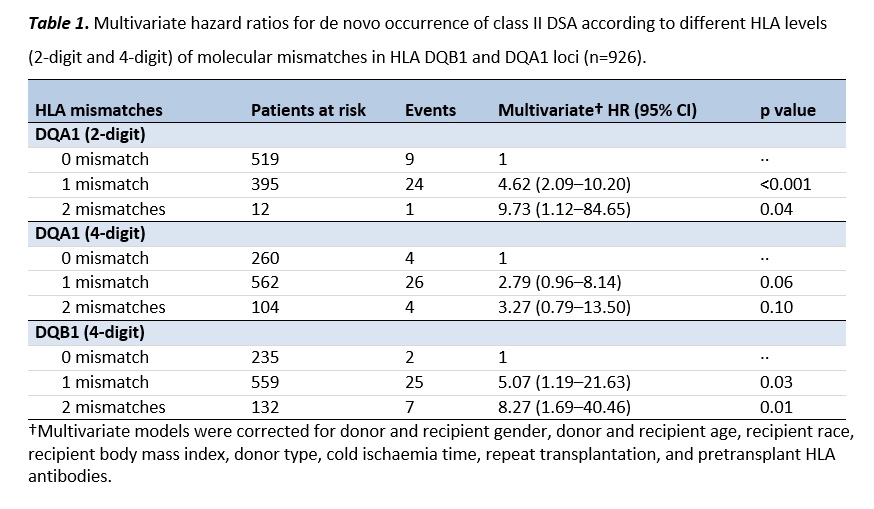
*Results: Our study cohort comprised mainly first single-kidney transplant recipients (86.7%) with mean age of 53.8 ±13.2 years, male (59.8%) and mainly Caucasians (98.4%). DnDSA occurred in 43 (4.6%) patients during the antibody follow-up. Multivariate Cox regression analysis showed an independent association between antibody-verified eplet mismatch load and dnDSA occurrence (HR 1.06/mismatch, 95%CI 1.02-1.10;p=0.002), fully explained by DQ antibody-verified eplet effects (HR 1.14/mismatch, 95%CI 1.07-1.22;p<0.001). The association with DQ antibody-verified eplet mismatches was linear, without a safe threshold at which DSA did not occur. Given this linearity, we investigated which MM in the two different DQA1 and DQB1 loci were independently associated with HLA class II dnDSA (Table 1). Besides one (HR=5.07, 95%CI 1.19-21.63;p=0.03) and two (HR=8.27, 95%CI 1.69-40.46;p=0.01) 4-digit DQB1 MM, one and two 2-digit mismatches for DQA1 were also independently associated in multivariate analysis with class II dnDSA occurrence (HR=4.62, 95% CI 2.09-10.20; p<0.001 and HR=9.73, 95% CI 1.12-84.65; p=0.04, respectively).This suggests that the α chain has an important role in the immunogenicity of the DQ molecule and indicates the importance of considering both DQA1 and DQB1 mismatches for minimizing dnDSA occurrence. This can be best achieved by 2-digit and 4-digit DQA1/DQB1 matching, respectively.
*Conclusions: Antibody-verified eplet mismatches in HLA-DQ, but no other HLA loci confer substantial risk for dnDSA after kidney transplantation. Our findings indicate that adding molecular DQA1/DQB1 matching to the current antigen HLA-A,-B,-DR matching algorithm will decrease dnDSA formation after transplantation.
To cite this abstract in AMA style:
Senev A, Coemans M, Sandt VVan, Loon EVan, Callemeyn J, Sprangers B, Kuypers D, Emonds M, Naesens M. The Impact of HLA-DQ Molecular Mismatches on De Novo Occurrence of Donor-Specific Anti-HLA Antibodies after Kidney Transplantation: An Observational Cohort Study [abstract]. Am J Transplant. 2020; 20 (suppl 3). https://atcmeetingabstracts.com/abstract/the-impact-of-hla-dq-molecular-mismatches-on-de-novo-occurrence-of-donor-specific-anti-hla-antibodies-after-kidney-transplantation-an-observational-cohort-study/. Accessed May 27, 2026.« Back to 2020 American Transplant Congress