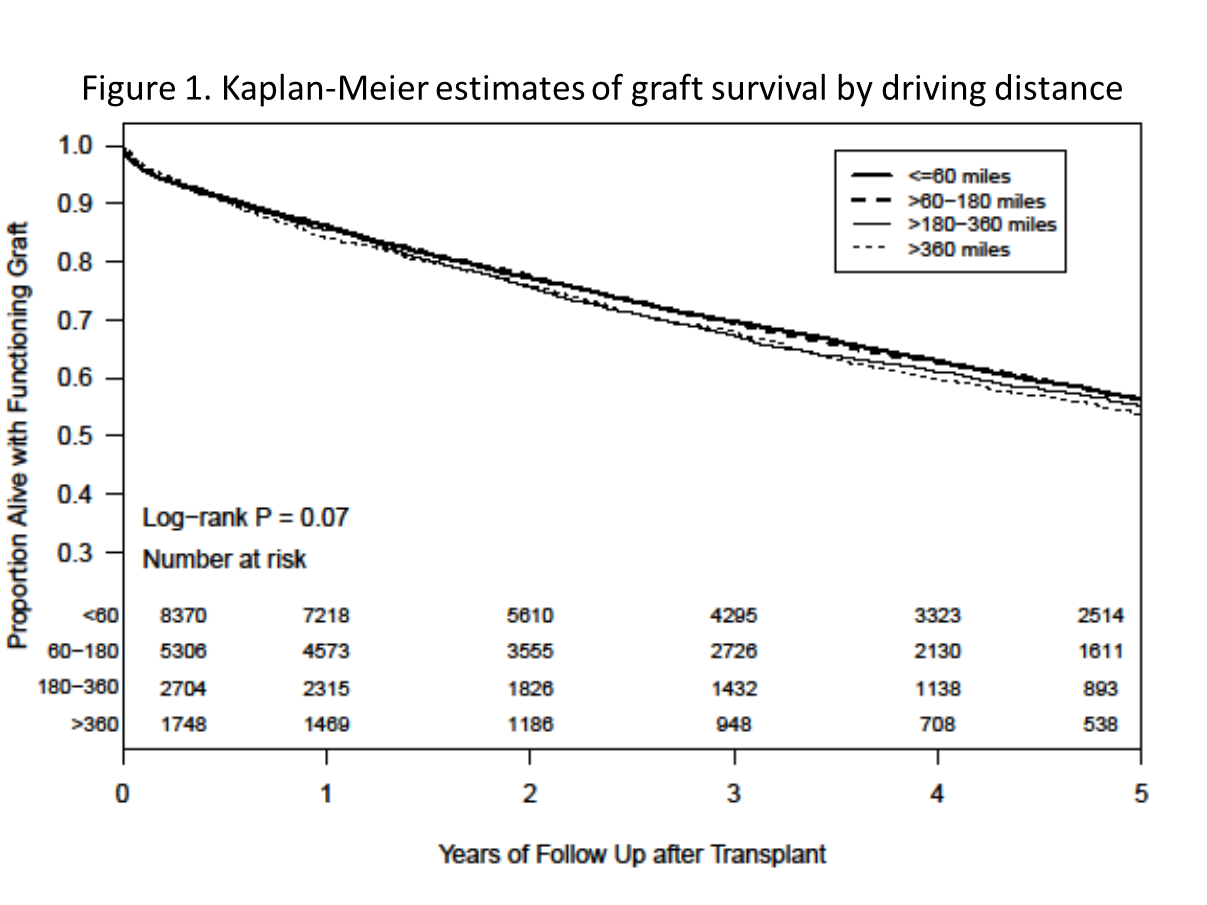
The Burden of Recipient Driving Distance and Post Lung Transplant Outcomes: A National Cohort Study
Cleveland Clinic, Cleveland, OH
Meeting: 2019 American Transplant Congress
Abstract number: 188
Keywords: Lung, Lung transplantation
Session Information
Session Name: Concurrent Session: Setting the Table for Success after Lung Transplantation
Session Type: Concurrent Session
Date: Sunday, June 2, 2019
Session Time: 4:30pm-6:00pm
 Presentation Time: 4:42pm-4:54pm
Presentation Time: 4:42pm-4:54pm
Location: Room 206
*Purpose: There are only 75 lung transplant centers in the United States, which leads to a spectrum of travel burdens among patients in order to access care. Travel burdens include repeated travel from home to transplant center for a lifetime of post-transplant visits, and the impact on long term outcomes is unknown. Our hypothesis was that longer travel burden, measured as driving distance in miles from household zip code to transplant center, was not associated with lower post-transplant graft survival.
*Methods: Retrospective national cohort study of all adult first time lung only transplants in the United States listed and transplanted between January 1, 2006 through May 31, 2017, and reported to the Scientific Registry of Transplant Recipients. Patients traveling from outside the U.S. were excluded. Driving distance was determined from the patient’s household zip code to the transplant center using SAS URL access to GoogleMaps. Distance was categorized as <=60, >60-180, >180-360, and >360 miles. Kaplan-Meier survival analysis and adjusted Cox proportional hazard models were used to assess the relationship between patient driving distance and graft survival.
*Results: 18,128 patients met inclusion criteria. The median driving distance was 69.6 miles. 46.2% (8,370) drove <=60 miles to the transplant center, 29.3% (5,306) drove >60-180 miles, 14.9% (2,704) drove >180-360 miles, and 9.6% (1,748) drove >360 miles. 22.5% of the study cohort drove more than 60 miles from home and bypassed the nearest transplant center to seek care at a more distant center. Patients with the furthest driving distance were significantly more likely to be male (63.2% vs 58.3% in <60), have a higher lung allocation score (mean 49.8 vs. 47.4 for <60), shorter waitlist time (median 36 days vs 63 for <60), a higher likelihood of acute rejection in the first year after transplant (29.2% vs 20.4% in <60), and less likely to receive a donation after cardiac death donor (1.6% vs 2% in <60). In both Kaplan-Meier (see figure 1) and adjusted models there was no significant difference in long term graft survival.
*Conclusions: While post-transplant graft survival was not significantly different by driving distance, longer travel distance was associated with a higher likelihood of acute rejection within the first year after transplant. One fifth of patients sought care at a more distant center. Further work is necessary to understand the impact of recipient travel distance on outcomes such as quality of life and out of pocket travel costs.
To cite this abstract in AMA style:
Tsuang W, Arrigain S, Lopez R, Snair M, McCurry K, Budev M, Schold J. The Burden of Recipient Driving Distance and Post Lung Transplant Outcomes: A National Cohort Study [abstract]. Am J Transplant. 2019; 19 (suppl 3). https://atcmeetingabstracts.com/abstract/the-burden-of-recipient-driving-distance-and-post-lung-transplant-outcomes-a-national-cohort-study/. Accessed May 23, 2026.« Back to 2019 American Transplant Congress