Superior Metabolic Function of Type 2 Diabetes Mellitus Patients After Simultaneous Kidney/pancreas Transplantation Compared with Kidney Transplantation Alone
X. Y. Fu, C. Yu, H. Wang, J. Zhao, Z. Wang, C. Mo, X. Shi, G. Feng, W. Song, Z. Shen
Tianjin First Centeral Hospital, Tianjin, China
Meeting: 2021 American Transplant Congress
Abstract number: 896
Keywords: Graft survival, Kidney/pancreas transplantation, Metabolic disease, Renal function
Topic: Clinical Science » Kidney » Kidney: Cardiovascular and Metabolic Complications
Session Information
Session Name: Kidney: Cardiovascular and Metabolic Complications
Session Type: Poster Abstract
Session Date & Time: None. Available on demand.
Location: Virtual
*Purpose: To compare the renal function, metabolic profiles and survival outcomes of simultaneous pancreas kidney transplantation (SPK) and kidney transplantation alone (KTA) to end-stage renal disease (ESRD) patients with type II diabetes mellitus (T2DM).
*Methods: patients with ESRD combined with T2DM who underwent SPK (n=85) or KTA (n=71) in our center were retrospectively analyzed. General demography data, perioperative parameters, postoperative blood glucose and lipid profiles, complications and survival outcomes in these two cohorts were analyzed. Repeated data were compared with mixed effect model.
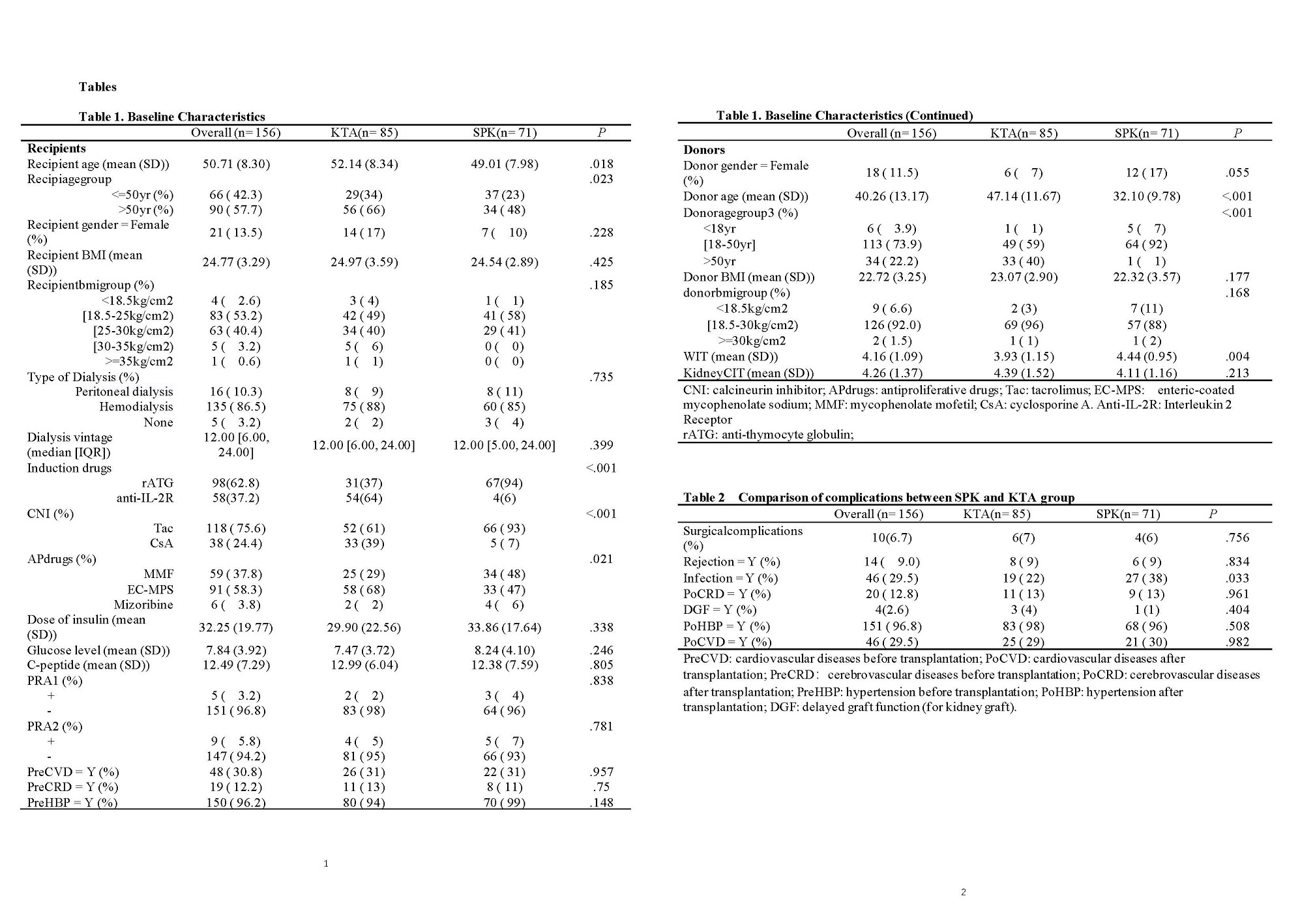
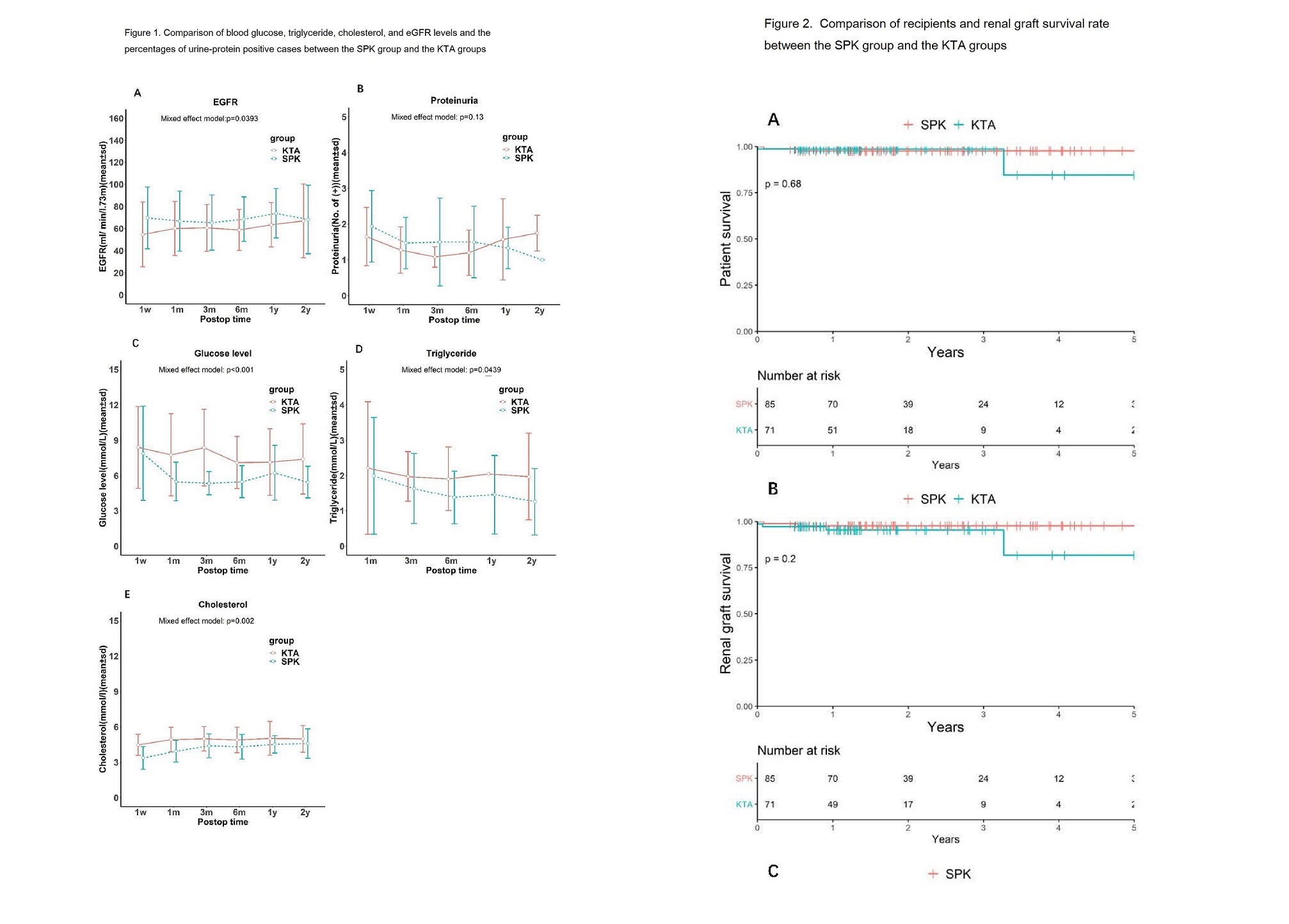
*Results: SPK recipients were generally younger than KTA recipients (49.01±7.98 vs. 52.14±8.34 years, p = 0.018), as well as for the age of donors (32.1±9.78 vs. 47.14±11.67 years, p <0.001)(Table1). SPK leads to superior renal function and metabolic outcomes, with higher eGFR level (p=0.393), lower fasting serum glucose level (p<0.001), lower triglyceride level (p =0.0439), and lower cholesterol level (p=0.002) (Figure 1). The rate of infection was higher in KTA group (38% vs. 22.4% , p = 0.003) (Table2). The survival outcomes were comparable between the two groups(Figrue2).
*Conclusions: SPK provides better renal function and metabolic outcomes, but has higher rate of infection than KTA for ESRD-T2DM patients. The 5-year survival outcomes of recipients and grafts were comparable between the two groups.
To cite this abstract in AMA style:
Fu XY, Yu C, Wang H, Zhao J, Wang Z, Mo C, Shi X, Feng G, Song W, Shen Z. Superior Metabolic Function of Type 2 Diabetes Mellitus Patients After Simultaneous Kidney/pancreas Transplantation Compared with Kidney Transplantation Alone [abstract]. Am J Transplant. 2021; 21 (suppl 3). https://atcmeetingabstracts.com/abstract/superior-metabolic-function-of-type-2-diabetes-mellitus-patients-after-simultaneous-kidney-pancreas-transplantation-compared-with-kidney-transplantation-alone/. Accessed May 20, 2026.« Back to 2021 American Transplant Congress