Should Steatotic Livers Be Transplanted Into Pediatric Recipients?
UT Southwestern, Dallas, TX
Meeting: 2020 American Transplant Congress
Abstract number: D-272
Keywords: Biopsy, Donors, marginal, Liver transplantation, Weight
Session Information
Session Name: Poster Session D: Biomarkers, Immune Assessment and Clinical Outcomes
Session Type: Poster Session
Date: Saturday, May 30, 2020
Session Time: 3:15pm-4:00pm
 Presentation Time: 3:30pm-4:00pm
Presentation Time: 3:30pm-4:00pm
Location: Virtual
*Purpose: Although steatotic livers are frequently transplanted in the adult population, they are not commonly transplanted in pediatric recipients. We questioned if the outcomes of steatotic livers in pediatric recipients are comparable to non-steatotic livers and if increased utilization of these livers might be considered.
*Methods: We utilized the UNOS database to examine outcomes in all pediatric liver transplant recipients (>18 years) who were transplanted between 2006—2018. Recipients of living donor and multi-organ transplants were excluded. Livers were considered to be steatotic if a biopsy showed >5% macrosteatosis. Donor and recipient demographic data were examined, as were survival and outcomes data. A p-value of <0.05 was considered to be significant.
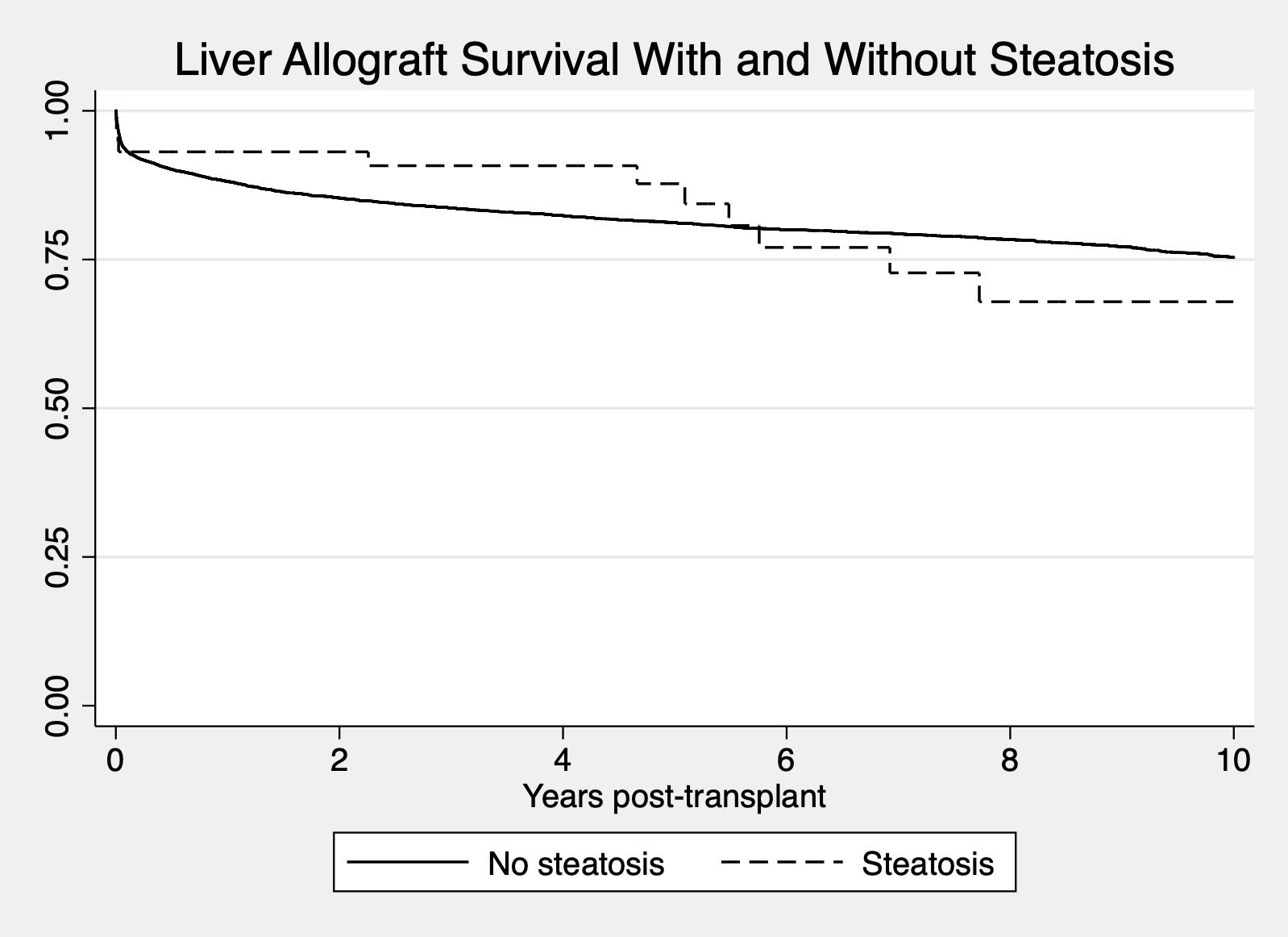
*Results: There were 7,311 pediatric liver transplants performed during the study period. 58 recipients received a steatotic liver while 7,253 were transplanted with a non-steatotic liver. Recipients of the steatotic livers were more likely to be older (8.8 vs. 5.0 years) have a higher final MELD/PELD score (21 vs. 14), and less likely to have had previous abdominal surgeries. There were no differences in BMI or length of stay. Donors with steatosis were older (27.1 vs. 11.3 years), had a greater BMI (25.2 vs. 19.7 kg/m2). Macrosteatosis in the steatosis livers was 17.5% vs. 1.4% in the non-steatotic livers. There were no differences in cold ischemia time, distance to transplant center, or transaminases. Allograft survival was also not significantly different between the two groups (Figure 1). Primary non-function, acute and chronic rejection, vascular thrombosis, and biliary complications were also similar between groups.
*Conclusions: Pediatric patients who receive biopsy proven steatotic livers have similar outcomes to those with non-steatotic livers. With appropriate donor and recipient selection the utilization of steatotic livers can be used to expand the pediatric donor pool with good short and long-term outcomes
To cite this abstract in AMA style:
MacConmara M, Feizpour C, Vagefi P, Ramirez C, DeGregorio L, Hwang CS. Should Steatotic Livers Be Transplanted Into Pediatric Recipients? [abstract]. Am J Transplant. 2020; 20 (suppl 3). https://atcmeetingabstracts.com/abstract/should-steatotic-livers-be-transplanted-into-pediatric-recipients/. Accessed May 24, 2026.« Back to 2020 American Transplant Congress