Post-Liver Transplant Metabolic Syndrome Increases the Risk of Recurrent Fibrosis in Patients With Hepatitis C
R. Sharma, M. Laurito, R. Brown, Jr., E. Verna.
Department of Medicine, Columbia University, New York, NY.
Meeting: 2015 American Transplant Congress
Abstract number: 225
Keywords: Fibrosis, Hepatitis C, Liver transplantation, Post-transplant diabetes
Session Information
Session Name: Concurrent Session: Liver Transplantation: Viral Hepatitis
Session Type: Concurrent Session
Date: Monday, May 4, 2015
Session Time: 2:15pm-3:45pm
 Presentation Time: 3:15pm-3:27pm
Presentation Time: 3:15pm-3:27pm
Location: Terrace IV
Introduction: Post-liver transplant (LT) metabolic syndrome (MS) is common and may impact fibrosis progression in LT recipients with hepatitis C virus (HCV). Methods: All adults with HCV and LT 9/07-6/13 were retrospectively assessed. MS was defined by US National Cholesterol Education Program Adult Treatment Panel III, including abnormalities in 3/5 parameters: triglycerides, HDL, glucose, blood pressure and waist circumference/BMI. The impact of MS on time to significant fibrosis (F≥2 or cholestatic hepatitis) was assessed by Kaplan-Meier and proportional hazards. Protocol liver biopsies are performed at our center at 3 months then annually, as well as for cause. Those with negative HCV at LT, HBV, HIV or died within 3 months were excluded. Results: 156 patients were analyzed; mean age 57.1 years, 71% male, median (range) follow-up 4.5 (0.3-8.4) years. 22% never had MS, 55% had MS at LT, and 76% had MS at any time post-LT (63% < 1 year and 66% > 1 year post-LT). Patient characteristics were similar in those with and without post-LT MS including age, gender, race/ethnicity, HCC, immunosuppression (induction, calcineurin inhibitor), proportion with acute rejection, post-LT HCV treatment or SVR, and median follow-up. Patients with post-LT MS were more likely to have pre-LT MS (p<0.001), DM (p<0.001) and hypertension (p<0.001). Patients with post-LT MS were more likely to develop significant fibrosis (65%) than patients without post-LT MS (26%, p<0.001, see figure). In unadjusted analysis, post-LT MS (HR 3.34, p=0.001), female gender (1.65, p=0.03), and donor age (1.02, p=0.02) predicted significant fibrosis, and remained significant in the final adjusted model: post-LT MS (3.96, p=0.001), female gender (1.72, p=0.04), donor age (1.02, p=0.01). There was a non-significant trend towards increased mortality in patients with post-LT MS (32%) compared to those without (20%, p=0.17). Conclusions: Post-LT MS affects the majority of LT recipients with HCV (76%), and leads to a >3-fold increase in the risk of recurrent significant fibrosis. Identification and modification of MS risk factors may be essential to improving post-LT outcomes.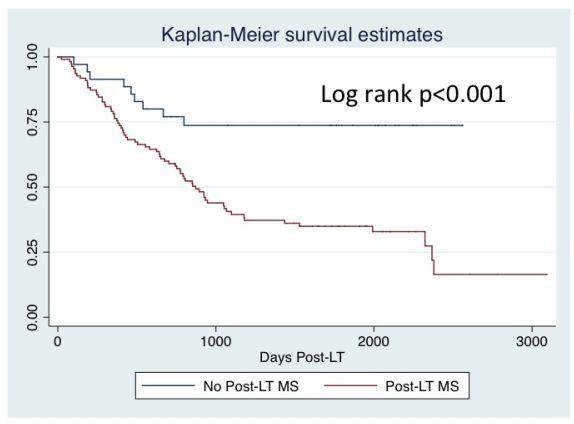
To cite this abstract in AMA style:
Sharma R, Laurito M, Brown R, Verna E. Post-Liver Transplant Metabolic Syndrome Increases the Risk of Recurrent Fibrosis in Patients With Hepatitis C [abstract]. Am J Transplant. 2015; 15 (suppl 3). https://atcmeetingabstracts.com/abstract/post-liver-transplant-metabolic-syndrome-increases-the-risk-of-recurrent-fibrosis-in-patients-with-hepatitis-c/. Accessed May 17, 2026.« Back to 2015 American Transplant Congress
