National Trends in Locoregional Therapy among Liver Transplant (LT) Candidates with Hepatocellular Carcinoma (HCC) in the United States
1Stanford University, Redwood City, CA, 2University of California, San Francisco, San Francisco, CA
Meeting: 2020 American Transplant Congress
Abstract number: 147
Keywords: Hepatocellular carcinoma, Liver, Liver transplantation, Waiting lists
Session Information
Session Name: Liver: Hepatocellular Carcinoma and Other Malignancies I
Session Type: Oral Abstract Session
Date: Saturday, May 30, 2020
Session Time: 3:15pm-4:45pm
 Presentation Time: 3:51pm-4:03pm
Presentation Time: 3:51pm-4:03pm
Location: Virtual
*Purpose: Advances in locoregional therapy (LRT) have expanded treatment options for patients with HCC. As recent policy changes in the United States (US) have lengthened waiting times for patients with HCC, an increasing proportion receive LRT as bridging therapy prior to LT. The aim of this study was to investigate temporal trends in LRT among LT candidates in the US.
*Methods: Data for all primary adult LT candidates listed from 2003 and 2018 who received an HCC exception were extracted from the national US registry. The date and type of LRT, if any, was reported with each submitted HCC exception application. Combination therapy (i.e. ablation + chemoembolization or radioembolization) was defined as receipt of these therapies within 30 days. Linear regression models were used to evaluate variables that were associated with greater number of treatments. Multivariable Cox regression analysis was used to evaluate the association between type of LRT and waitlist dropout, defined by removal from the list for death or being too sick.
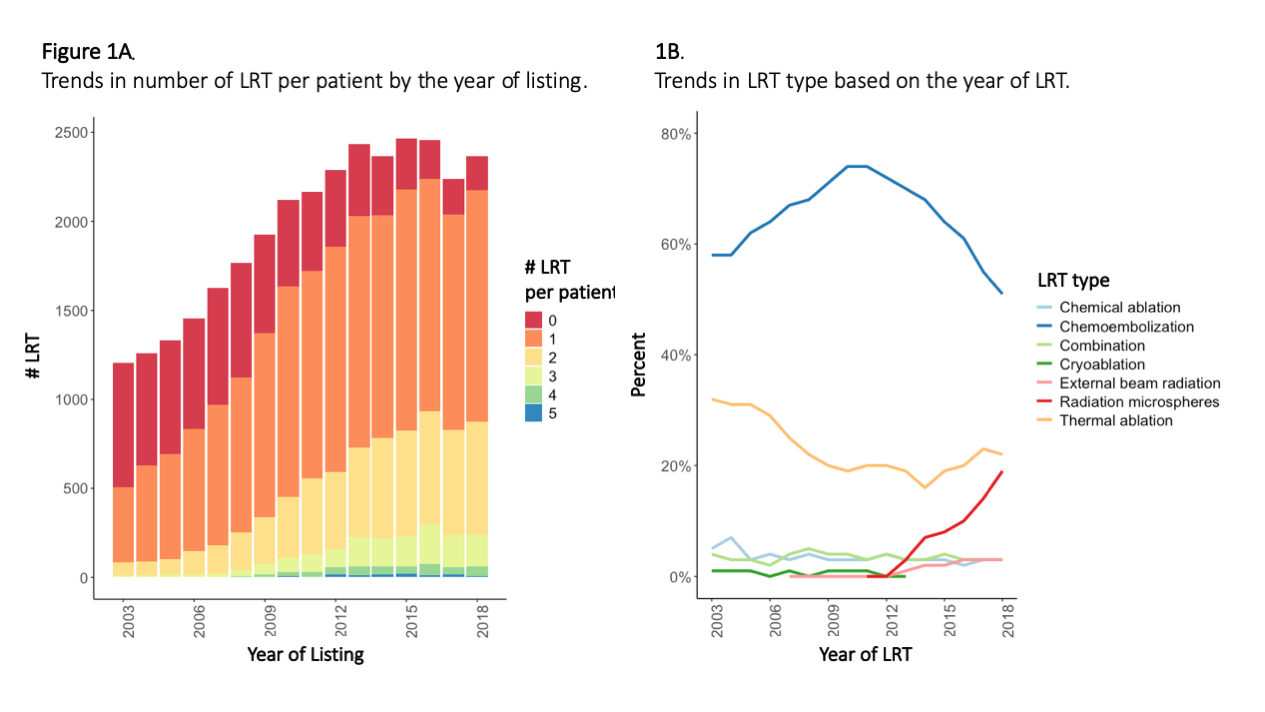
*Results: There were 31,464 eligible patients with at least one approved HCC exception application. In total, there were 34,445 treatments among 24,031 LT candidates. The proportion of patients with at least one LRT recorded increased from 42.1% in 2003 to 92.0% in 2018. Figure 1 demonstrates trends in number of treatments per patient by year of listing, and treatment type based on the year of treatment. Chemoembolization remains the most frequent type of LRT, followed by ablation. However, there has been a notable increase in radioembolization in the past 5 years, now making up 19% of LRT in 2018, compared to <5% as recently as 2013. Initial HCC outside T2 criteria, AFP > 500, Child-Pugh class A, lower MELD, and listing in longer wait time regions was associated with a greater number of liver-directed treatments while awaiting LT (p<0.05 for all). In the multivariable Cox regression analysis, adjusting for AFP, Child-Pugh class, MELD, wait time region, and year of listing, receipt of LRT was associated with a lower risk of waitlist dropout, including chemoembolization (HR 0.85), ablation (HR 0.74), external beam radiation (HR 0.62), and radioembolization (HR 0.85) (p<0.05 for all).
*Conclusions: In the US, LRT — and in particular radioembolization — is increasingly used to bridge to LT. Patients with HCC outside T2 criteria and those with more compensated liver disease undergo more treatments while awaiting LT. Receipt of LRT is associated with a lower risk of waitlist dropout.
To cite this abstract in AMA style:
Kwong A, Kim W, Yao F, Mehta N. National Trends in Locoregional Therapy among Liver Transplant (LT) Candidates with Hepatocellular Carcinoma (HCC) in the United States [abstract]. Am J Transplant. 2020; 20 (suppl 3). https://atcmeetingabstracts.com/abstract/national-trends-in-locoregional-therapy-among-liver-transplant-lt-candidates-with-hepatocellular-carcinoma-hcc-in-the-united-states/. Accessed June 2, 2026.« Back to 2020 American Transplant Congress