Leukopenia in the Renal Transplant Population
1Emory University, Atlanta, GA, 2Surgery, Emory University, Atlanta, GA
Meeting: 2021 American Transplant Congress
Abstract number: 646
Keywords: Immunosuppression, Kidney transplantation, Leukocytes, Outcome
Topic: Clinical Science » Biomarkers, Immune Assessment and Clinical Outcomes
Session Information
Session Name: Biomarkers, Immune Assessment and Clinical Outcomes
Session Type: Poster Abstract
Session Date & Time: None. Available on demand.
Location: Virtual
*Purpose: Leukopenia is a common complication for transplant patients on immunosuppression, but etiologies, timing, and outcomes are only superficially understood.
*Methods: All patients undergoing kidney transplant at Emory University Hospital between the years 2009 and 2019 were included. Using CTCAE definitions, moderate leukopenia was defined as lowest white blood cell (wbc) value between 1 and 2, and severe leukopenia was defined as lowest wbc <1. We explored longitudinal measures of leukopenia to determine the relevance of patterns of wbc levels. Longitudinal leukopenia was measured by the integral of 2-wbc over the first year post transplant, representing the amount of time the patient spent with a white blood cell count of less than 2. This AUC (area under the curve) was adjusted for length of follow-up, multiplying by a factor of 365/days of follow-up. Survival and graft loss at 3 years post transplant was analyzed in the context of these two different measures.
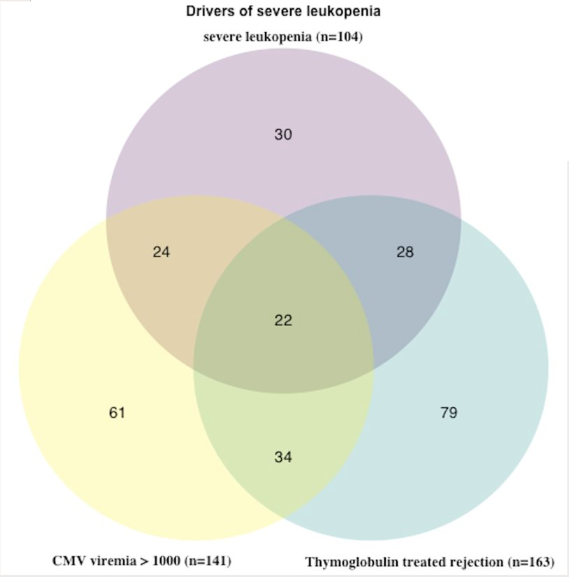
*Results: Of 2059 patients, 61% were on belatacept and 39% on tacrolimus immunosuppression. 104 patients had severe and 367 had significant leukopenia. Age, sex, race, and etiology of renal disease were equally balanced between groups. Patients with significant or severe leukopenia were more likely to have received a kidney from a deceased donor, to be CMV high risk, and to be on immunosuppression with tacrolimus or azathioprine. On multivariate regression controlling for donor type, azathioprine use, and cmv risk status, immunosuppression with tacrolimus was no longer associated with leukopenia. 62% of patients with severe leukopenia experienced CMV viremia, while 48% had undergone treatment with thymoglobulin. Thirty patients had severe leukopenia not explained by CMV viremia or prior thymoglobulin treatment. When quantified using CTCAE definitions, 24% of patients with severe leukopenia versus 19% of patients with significant leukopenia, and 8% of patients without leukopenia experienced graft loss or death at 3 years. Surprisingly, for significant and severe patients, AUC was not significantly associated with graft loss or death.
*Conclusions: While there are significant differences in protective immunity for patients on belatacept and tacrolimus, the incidence of leukopenia in these populations does not appear to be different. In our patients, leukopenia in the first year transplant was associated with increased rates of graft loss and death, underscoring the need to develop management pathways for these at-risk patients. Further study is warranted to understand this population.
To cite this abstract in AMA style:
Johnson A, Karadkhele G, Larsen C. Leukopenia in the Renal Transplant Population [abstract]. Am J Transplant. 2021; 21 (suppl 3). https://atcmeetingabstracts.com/abstract/leukopenia-in-the-renal-transplant-population/. Accessed May 23, 2026.« Back to 2021 American Transplant Congress