Impact of Ozone Exposure of Lung Donors and Recipients on All-Cause Mortality after Lung Transplant
1Surgery, UNC at Chapel Hill, Chapel Hill, NC, 2Institute of the Environment, UNC at Chapel Hill, Chapel Hill, NC
Meeting: 2020 American Transplant Congress
Abstract number: 85
Keywords: Lung, Lung transplantation, Outcome, Survival
Session Information
Session Name: From Bench to Community to Bedside in Lung Transplantation
Session Type: Oral Abstract Session
Date: Saturday, May 30, 2020
Session Time: 3:15pm-4:45pm
 Presentation Time: 3:51pm-4:03pm
Presentation Time: 3:51pm-4:03pm
Location: Virtual
*Purpose: A Belgian study found proximity to a motorway increased risk of bronchiolitis obliterans syndrome after lung transplant (LT). Using zip codes as a surrogate for habitat location, we investigated the impact of ozone exposure of donors and recipients on mortality after LT in the US.
*Methods: UNOS Standard Transplant Analysis and Research (STAR) database (June 30, 2017) identified adult LT recipients and their donors between 2005 and 2015, and their zip code of residence at LT. Daily maximum 8-hour average ozone concentration (MDA8O3) associated with donor and recipient residencies 1 year prior to and after LT respectively, were estimated by mapping each zip code to a census tract, using a crosswalk from HUD, downscaled from a 12×12-km sq grid resolution detailed chemistry – transport model application using a Bayesian space-time downscaler, and then fused with surface observations. Ozone concentration was classified into low (<35 parts/billion (ppb)), medium (35-42 ppb) and high (>42 ppb) exposure categories. Cox proportional hazards regression and Kaplan-Meier curves assessed the impact of ozone on 1-year and long-term all-cause mortality.
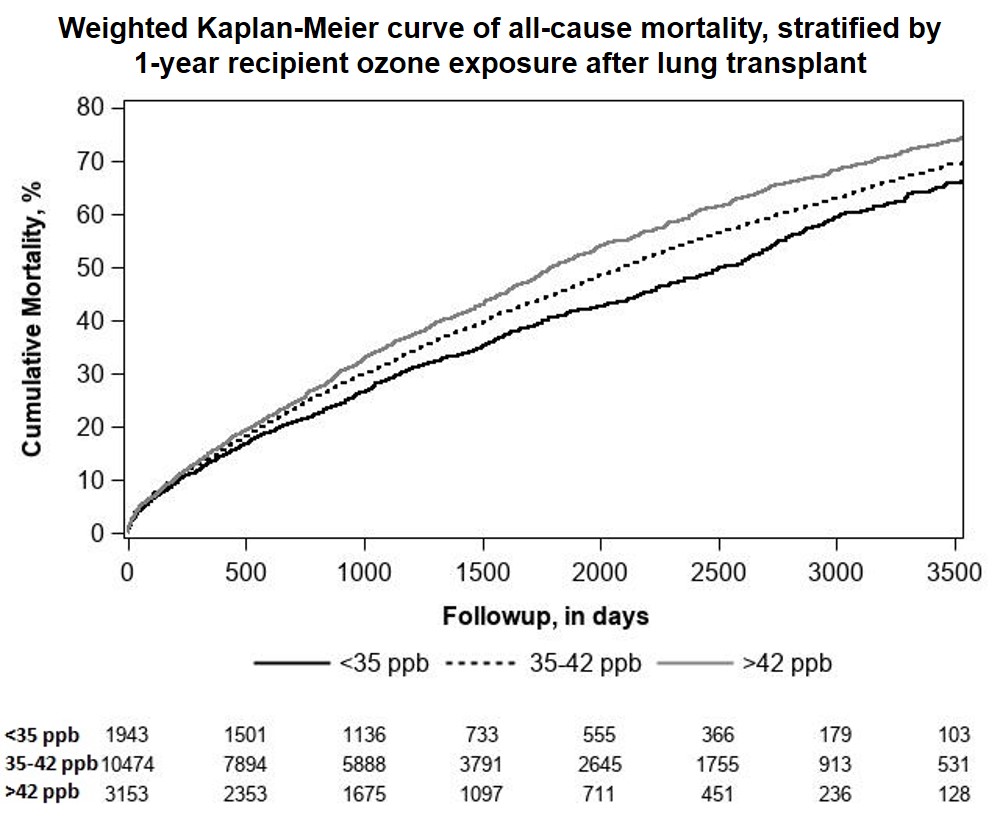
*Results: 17,760 LT were analyzed. Median follow-up was 1101 days (IQR 511-2073, range 1-4448). 22% of LT had high donor exposure and 20% had high recipient exposure. Recipient ozone exposure after LT had minimal impact on 1-year mortality; however, higher ozone concentration was associated with increased all-cause mortality (Figure). Compared to low exposure, medium (HR 1.13, 95% CI 1.05, 1.22) and high (HR 1.28, 95% CI 1.17, 1.40) both increased patient risk of death. Donor ozone exposure in the year before LT did not appear to impact LT outcomes (Table).
*Conclusions: Ozone exposure is associated with increased long-term risk of death after LT. Ozone is only one aspect of air quality. Additional research on other air quality measures focusing on traffic-related air pollutants is needed.
| Donor Exposure | Recipient Exposure | ||||
| HR (95% CI)a | p-value | HR (95% CI)a | p-value | ||
| 1-year mortality | Low (for both) | ref | ref | ||
| Medium | 1.18 (1.02, 1.35) | 0.02 | 1.07 (0.92, 1.23) | 0.39 | |
| High | 0.99 (0.84, 1.17) | 0.92 | 1.15 (0.98, 1.35) | 0.09 | |
| Long-term mortality | Medium | 1.05 (0.97, 1.13) | 0.21 | 1.13 (1.05, 1.22) | 0.002 |
| High | 1.06 (0.98, 1.16) | 0.15 | 1.28 (1.17, 1.40) | <0.0001 | |
| Abbreviations: HR, hazard ratio; CI, confidence interval. a Inverse-probability of treatment weights were used to account for potential confounding; weights included recipient age, gender, race/ethnicity, primary payer, total days on waitlist, single vs. double lung transplant, status at transplant (ICU, hospitalized, at home), life support (ventilator and ECMO), recipient and donor cigarette history, donor cause of death, and year of transplant. | |||||
To cite this abstract in AMA style:
Egan T, Arunachalam S, Chang C, Strassle P. Impact of Ozone Exposure of Lung Donors and Recipients on All-Cause Mortality after Lung Transplant [abstract]. Am J Transplant. 2020; 20 (suppl 3). https://atcmeetingabstracts.com/abstract/impact-of-ozone-exposure-of-lung-donors-and-recipients-on-all-cause-mortality-after-lung-transplant/. Accessed May 17, 2026.« Back to 2020 American Transplant Congress