Deceased-Donor Acute Kidney Injury Associates with Less BK Viremia in Kidney Transplant Recipients
For the DDS Consortium, Baltimore, MD
Meeting: 2019 American Transplant Congress
Abstract number: 531
Keywords: Donors, marginal, Kidney transplantation, Multicenter studies, Polyma virus
Session Information
Session Name: Concurrent Session: Kidney: Polyoma
Session Type: Concurrent Session
Date: Tuesday, June 4, 2019
Session Time: 4:30pm-6:00pm
 Presentation Time: 4:54pm-5:06pm
Presentation Time: 4:54pm-5:06pm
Location: Ballroom B
*Purpose: BK viremia (BKV) and polyomavirus nephropathy are kidney transplant complications that contribute to morbidity and graft loss, and prior studies suggest they may be donor derived, are likely due to over immunosuppression, and may be influenced by peri-transplant processes that disrupt allograft integrity. We hypothesized that donor AKI, which is associated with kidney discard and delayed graft function, could also be a risk factor for BKV post-transplant because of early tubular injury in the allograft.
*Methods: Between 2010 and 2013, we enrolled over 1600 donors into the multicenter, prospective Deceased-Donor Study. We recorded outcomes for 1030 recipients of these donor kidneys via detailed chart review at 13 transplant centers and fit Cox regression models for 1) development of BKV (any detectable viremia) and 2) a composite of BKV, all-cause graft failure or eGFR <20 ml/min/1.73m2 (both outcomes within 1 year of transplant) with adjustment for donor, transplant and recipient factors.
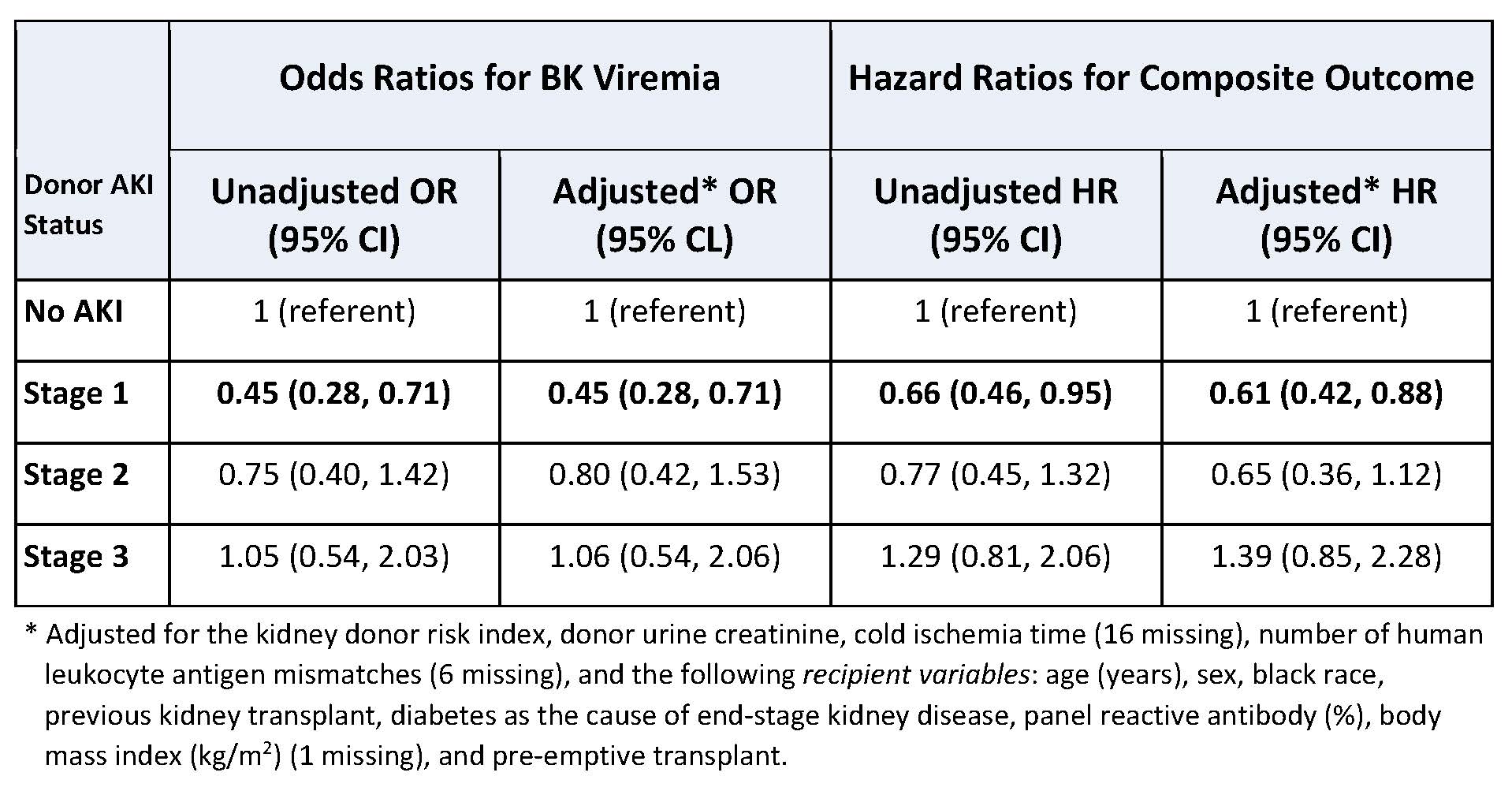
*Results: Mean±SD kidney donor profile index was 49±27% and 26% met serum creatinine criteria for AKI. Mean recipient age was 54±13 years, 61% were male and 46% were black. 25% of all recipients developed BKV, with 27% of non-AKI kidney recipients developing BKV compared with 18% of AKI kidney recipients (p=0.006). The composite outcome occurred in 31% of all recipients, 35% of non-AKI kidney recipients and 28% of AKI kidney recipients (p=0.04). On multivariable adjustment, stage 1 donor AKI remained protective against both BKV and the composite outcome (figure).
*Conclusions: In this large and carefully phenotyped cohort, deceased-donor AKI was common but did not associate with increased risk for BKV or a composite outcome of BKV, graft failure or poor allograft function at 1 year. In fact, mild donor AKI was independently protective against this complication. While there is the potential for selection bias in that it is likely that centers preferentially selected better-quality AKI kidneys for transplant, these findings indicate the possibility that donor AKI induces morphological or immunological changes to the allograft that protect against BKV post-transplant except when donor AKI is severe. More research is needed to better understand these unexpected results
To cite this abstract in AMA style:
Hall IE, Reese PP, Mansour SG, Mohan S, Doshi MD, Jia Y, Thiessen-Philbrook HR, Akalin E, Harhay MN, Muthukumar T, Schröppel B, Singh P, Weng FL, Bromberg JS, Parikh CR. Deceased-Donor Acute Kidney Injury Associates with Less BK Viremia in Kidney Transplant Recipients [abstract]. Am J Transplant. 2019; 19 (suppl 3). https://atcmeetingabstracts.com/abstract/deceased-donor-acute-kidney-injury-associates-with-less-bk-viremia-in-kidney-transplant-recipients/. Accessed June 2, 2026.« Back to 2019 American Transplant Congress