Arterial Blood Pressure at Time of Liver Transplant (LT) Evaluation Correlates With Kidney Biopsy Findings in LT Candidates With Renal Dysfunction
Transplant, Mayo Clinic, Jacksonville, FL.
Meeting: 2015 American Transplant Congress
Abstract number: 55
Keywords: Allocation, Biopsy, Kidney/liver transplantation, Liver transplantation
Session Information
Session Name: Concurrent Session: Optimizing Renal Outcomes in Liver Transplantation
Session Type: Concurrent Session
Date: Sunday, May 3, 2015
Session Time: 2:15pm-3:45pm
 Presentation Time: 2:15pm-2:27pm
Presentation Time: 2:15pm-2:27pm
Location: Room 118-AB
Renal dysfunction is common in LT candidates; however, predicting post-LT renal recovery is sometimes difficult. Kidney biopsy is helpful in identifying reversible renal injury but is associated with significant risks.
Aim: identify non-invasive method to predict post-LT renal recovery.
Methods:129 LT candidates with renal dysfunction of unknown cause (defined as iothalamate GFR <40 ml/min) and/or proteinuria underwent percutaneous kidney biopsy at time of LT evaluation. Patients with ≥30% interstitial fibrosis (IF) and/or ≥30-40% glomerulosclerosis (GS) were listed for simultaneous liver-kidney transplantation (SLK) while patients with lesser degrees of IF/GS were listed for LT alone. Prior to kidney biopsy, 24-hr urine protein and sodium excretions along with systolic and diastolic blood pressures (SBP and DBP, respectively) were measured. The use of anti-hypertensive medications other than diuretics was recorded.
Results: 73 (57%) patients were listed for LT and 56 were listed for SLK. Table 1 lists the clinical and histological findings of the 2 groups.
| Listed for LT n=73 | Listed for SLK n=56 | P | |
| %GS | 15±13 | 37±16 | 0.0001 |
| %IF | 9±5 | 25±14 | 0.0001 |
| Age (yr) | 59±7 | 60±8 | 0.3 |
| % male | 71 | 62 | 0.3 |
| % Hepatitis C | 41 | 44 | 0.4 |
| % previous LT | 17 | 29 | 0.3 |
| % Diabetes mellitus | 22 | 25 | 0.1 |
| % on BP medications | 9 | 27 | 0.01 |
| Iothalamate GFR (ml/min) | 30±17 | 26±11 | 0.1 |
| % dialysis at biopsy | 16 | 14 | 0.7 |
| 24-hr urine protein (mg/d)* | 56 (0-5406) | 135 (0-5604) | 0.2 |
| 24-hr urine sodium (mEq/d)* | 57 (0-289) | 76 (0-238) | 0.3 |
| SBP (mmHg) | 110±20 | 123±20 | 0.001 |
| DBP (mmHg) | 63±11 | 69±10 | 0.007 |
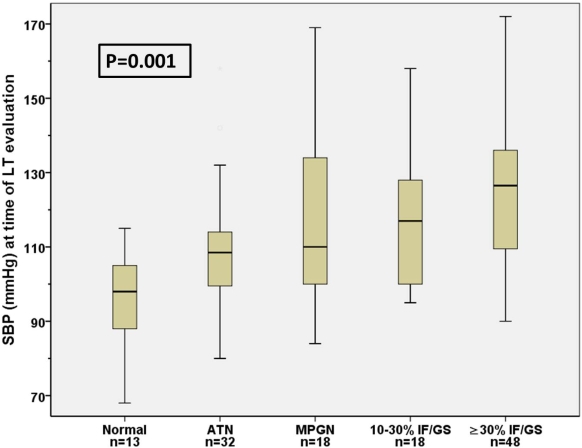 Conclusions: In LT candidates with renal dysfunction: 1)arterial BP in the low-normal range correlated with histological evidence of reversible renal injury 2) Anti-hypertensive medication use was associated with a higher likelihood of irreversible renal damage.
Conclusions: In LT candidates with renal dysfunction: 1)arterial BP in the low-normal range correlated with histological evidence of reversible renal injury 2) Anti-hypertensive medication use was associated with a higher likelihood of irreversible renal damage.
To cite this abstract in AMA style:
Wadei H, Peguero A, Alsaad A, Mai M, Oshel K, Gonwa T, Taner C, Keaveny A. Arterial Blood Pressure at Time of Liver Transplant (LT) Evaluation Correlates With Kidney Biopsy Findings in LT Candidates With Renal Dysfunction [abstract]. Am J Transplant. 2015; 15 (suppl 3). https://atcmeetingabstracts.com/abstract/arterial-blood-pressure-at-time-of-liver-transplant-lt-evaluation-correlates-with-kidney-biopsy-findings-in-lt-candidates-with-renal-dysfunction/. Accessed June 2, 2026.« Back to 2015 American Transplant Congress
