Surgical Error: A Common, Preventable Threat to Deceased Donor Organs
1New York Organ Donor Network, New York, NY
2Westchester Medical Center, Valhalla, NY
3Mount Sinai School of Medicine, New York, NY
4Columbia Presbyterian Medical Center, New York, NY.
Meeting: 2015 American Transplant Congress
Abstract number: 17
Keywords: Cadaveric organs, Donation, Hepatic artery, Renal injury
Session Information
Session Name: Concurrent Session: Deceased Donor Management
Session Type: Concurrent Session
Date: Sunday, May 3, 2015
Session Time: 2:15pm-3:45pm
 Presentation Time: 3:03pm-3:15pm
Presentation Time: 3:03pm-3:15pm
Location: Room 119-A
Deceased donor procurements (N = 340) performed through a single organ procurement organization during a 19 month period from 7/1/13 – 11/30/14 were reviewed through the performance improvement plan. Surgical errors were identified by anecdotal reports from recovery surgeons, perfusionists +/or transplanting surgeons.
A total of 34 errors were reported in 3 livers and 29 kidneys. One error involved an esophageal laceration and another involved retention of a foreign body following organ recovery. Errors were attributed to attending surgeons in 11/34 (33%), surgical fellows in 22/34 (65%) and a perfusionist in 1/34 (2%). 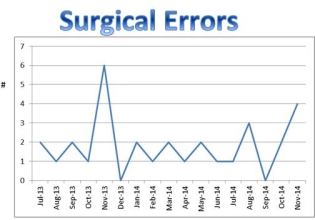
Renal injuries involved one or more arteries in 19/29 (66%), the ureter in 8/29 (28%) and a biopsy in 1/29 (3%). Two of three hepatic injuries involved the arterial supply to the organs. The mean BMI of donors in whom errors occurred was 31.0 vs. 27.6 for a group of 236 control donors. Overall, 22 of 34 errors (65%) were associated with successful transplantation.
We conclude that surgical errors occur during deceased donor procurements at a rate of approximately 1 in 10 donors despite the participation of multiple operators including both trainee and experienced surgeons. Most reported errors involved kidneys. Of these, the majority were arterial in nature. Approximately one third of these errors led to organ discards. Surgical error is an important and preventable cause of deceased donor organ loss. Efforts to avoid surgical error have become an important element of our PI plan and should be considered as a means of increasing the number of available organs from a limited pool of deceased donors.
To cite this abstract in AMA style:
Friedman A, Diflo T, Florman S, Ratner L, Marquez E, Tajik W. Surgical Error: A Common, Preventable Threat to Deceased Donor Organs [abstract]. Am J Transplant. 2015; 15 (suppl 3). https://atcmeetingabstracts.com/abstract/surgical-error-a-common-preventable-threat-to-deceased-donor-organs/. Accessed May 18, 2026.« Back to 2015 American Transplant Congress
