Successful Kidney Transplant Improves Glucose Tolerance – A Paradoxical Report From A Single Center
A. Mitsuke, H. Harada, H. Higuchi, N. Fukuzawa, H. Tanaka, T. Hirano, T. Sekii
Kidney Transplantation Surgery, Sapporo City General Hospital, Sapporo, Japan
Meeting: 2019 American Transplant Congress
Abstract number: C199
Keywords: Calcineurin, Kidney transplantation, Post-transplant diabetes, Weight
Session Information
Session Name: Poster Session C: Kidney: Cardiovascular and Metabolic
Session Type: Poster Session
Date: Monday, June 3, 2019
Session Time: 6:00pm-7:00pm
 Presentation Time: 6:00pm-7:00pm
Presentation Time: 6:00pm-7:00pm
Location: Hall C & D
*Purpose: Kidney recipients tend to impair glucose tolerance because of several factors such as post-operative obesity, and chronic exposure of some diabetogenic immunosuppressants like calcineurin inhibitors (CNI), corticosteroids (CS) and mTOR inhibitors (mTORi). The rate of new onset diabetes mellitus after transplantation (NODAT) has been reported in many literatures. However, the incidence varies presumably due to the difference of definition of NODAT and the vagueness of pre-transplant glucose tolerability. We herein surveyed the real incidence of NODAT using 75g OGTT method in our institution under early corticosteroid withdrawal or extremely minimization protocols.
*Methods: One hundred sixty-three kidney recipients without clinically diagnosed overt preoperative diabetes mellitus transplanted between 2006 to 2014, whose glucose tolerance (GT) were surveyed with 75g OGTT were enrolled. They were maintained with tacrolimus/mycofenolate mofetile based immunosuppression; their CS were discontinued at POD3 or continued with a minimum dose (2-4mg as methylprednisolone) by a month. Recent 33 patients were added with mTORi everolimus from the beginning. OGTT were performed before transplantation, and 1y post-transplant. Patients whose glucose at 2h lower 140mg/dL were diagnosed normal glucose tolerance (NGT), their glucose at 2h between 140 to 199mg/dL were ranked as impaired glucose tolerance (IGT), and their glucose at 2h more than 200mg/dL were defined as diabetes (DM). We also studied the change of body mass index(BMI) and insulinogenic tolerance or secretion using calculation of HOMA-R or HOMA-β.
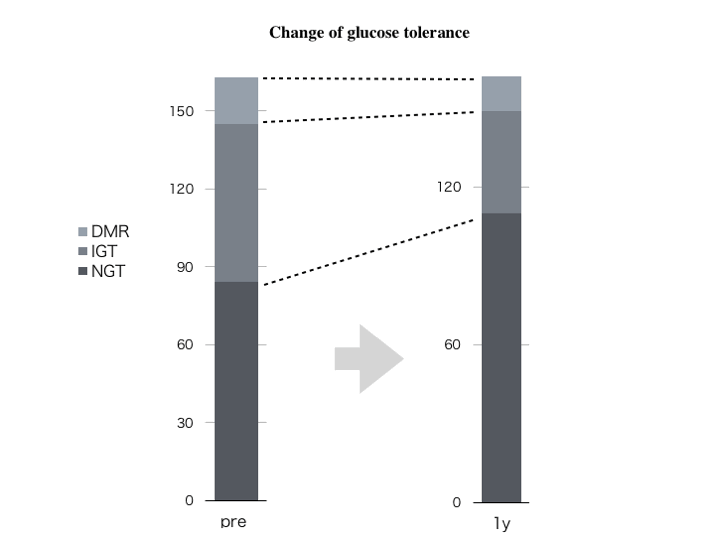
*Results: Out of 163 patients, pre-transplant latent DM were 18 (10.8%), IGT were 61 and rest 84 were in NGT. After 1y, 16 developed IGT, but 68 had never spoiled their GT in pre-transplant NGT patients. Among pre-operative IGT patients, 5 patients (8.2%) developed DM, 17 patients (27.9%) still remained their GT as IGT. Interestingly most of them could normalize their glucose intolerance (38, 62.3%). More interestingly, 10 patients out of 18 pre-transplant DM patients could recover their glucose tolerance at 1y (IGT 6, NGT 4) post-transplant. Then, the overall rate of real NODAT at 1y (DM at 1y / pre-operative IGT and NGT) were only 3.5% (5/143), or 14.7% (plus 16 IGT from 84 NGT) if included IGT patients. Patients who impaired their GT did not change their BMI. They exhibited the deterioration of HOMA-R not HOMA-β post-transplant.
*Conclusions: The real incidence of NODAT at 12m were extremely small different from previous literatures at least under maintenance early CS withdrawal or minimization protocol even with more diabetogenic CNI tacrolimus. More interestingly, it has been proven that GT could be recovered after successful kidney transplantation among clinically pre-operative non-diabetic population.
To cite this abstract in AMA style:
Mitsuke A, Harada H, Higuchi H, Fukuzawa N, Tanaka H, Hirano T, Sekii T. Successful Kidney Transplant Improves Glucose Tolerance – A Paradoxical Report From A Single Center [abstract]. Am J Transplant. 2019; 19 (suppl 3). https://atcmeetingabstracts.com/abstract/successful-kidney-transplant-improves-glucose-tolerance-a-paradoxical-report-from-a-single-center/. Accessed June 2, 2026.« Back to 2019 American Transplant Congress