Early Outcomes with the Liver-Kidney Safety Net
1University of Alabama at Birmingham, Birmingham, AL, 2University of Miami, Miami, FL
Meeting: 2020 American Transplant Congress
Abstract number: 369
Keywords: Allocation, Kidney transplantation, Liver transplantation, Survival
Session Information
Session Name: Liver Retransplantation and Other Complications
Session Type: Oral Abstract Session
Date: Saturday, May 30, 2020
Session Time: 3:15pm-4:45pm
 Presentation Time: 3:15pm-3:27pm
Presentation Time: 3:15pm-3:27pm
Location: Virtual
*Purpose: A safety net policy was implemented in August 2017 giving liver alone recipients with significant renal dysfunction post-transplant priority for subsequent renal transplantation. This study was undertaken to evaluate early outcomes under this policy.
*Methods: Adults who underwent isolated liver transplantation (LT) after implementation of the safety net policy on August 10, 2017 and were subsequently listed for kidney transplant (KT) between 60 and 365 days after liver transplantation contained in the March 2019 UNOS STAR file were studied. Outcomes of interest were receipt of a kidney transplant and post liver transplant survival. Survival in safety net patients was compared to isolated liver transplant recipients who were not subsequently listed for kidney transplant and survived at least 60 days post-transplant, adjusting for baseline covariates different between the two groups. Conditional survival after 60 days was chosen to reduce immortal time bias.
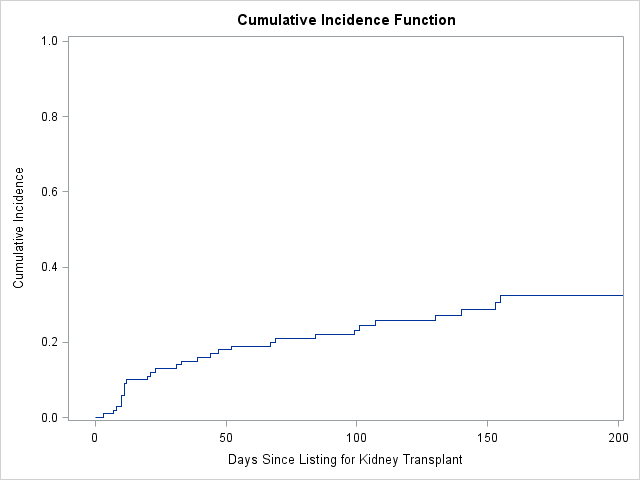
*Results: There were 9558 adults undergoing isolated LT in the study period, of whom 100 were subsequently listed for safety net KT during the study period, at a mean age of 56 and a mean GFR at LT of 34.3. Of these 100 patients, 60 were either on dialysis or had a GFR of 30 or less at LT, representing 3.7% of the 1603 patients in the larger study population transplanted on dialysis or with a GFR of 30 or less. The mean calculated MELD at LT for the safety net patients was 31.8. Notably, 12 safety net patients had a GFR over 60 at the time of liver transplantation. The median time to listing for KT was 212 days after liver transplant (IQR 145.5-296 days). The mean panel reactive antibody at listing was 8.5. The cumulative incidence of renal transplantation at 30, 60, and 180 days after listing was 13%, 19%, and 32.5% (figure). Patient survival after LT at 90, 180, and 365 days in the safety net group was 100%, 100%, and 95.5% vs. 99.2%, 97.7%, and 94.8% (p=0.809) for the comparison group. Adjusted for covariates, safety-net patients had statistically similar post-transplant survival to the comparison group (HR 0.675, 95% CI 0.248-1.834; p=0.441).
Figure: Cumulative incidence of kidney transplant for safety net patients. Time is in days from listing for kidney transplant. Death while waiting is treated as a competing risk.
*Conclusions: Conclusion: This early analysis suggests that the safety net policy functions well, providing rapid access to renal transplant and good survival for patients with prolonged renal insufficiency following liver transplantation.
To cite this abstract in AMA style:
Cannon RM, Goldberg DS, Eckhoff DE, Anderson DJ, Orandi BJ, Locke JE. Early Outcomes with the Liver-Kidney Safety Net [abstract]. Am J Transplant. 2020; 20 (suppl 3). https://atcmeetingabstracts.com/abstract/early-outcomes-with-the-liver-kidney-safety-net/. Accessed May 10, 2026.« Back to 2020 American Transplant Congress