Causes of Kidney Allograft Loss (GL) in the Current Era of Donor-Specific Alloantibody (DSA) Testing
1Mayo Clinic, Rochester, MN, 2Mayo Clinic, Scottsdale, AZ
Meeting: 2020 American Transplant Congress
Abstract number: 450
Keywords: Graft failure, Outcome, Survival
Session Information
Session Name: Kidney Complications: Immune Mediated Late Graft Failure
Session Type: Oral Abstract Session
Date: Saturday, May 30, 2020
Session Time: 3:15pm-4:45pm
 Presentation Time: 3:27pm-3:39pm
Presentation Time: 3:27pm-3:39pm
Location: Virtual
*Purpose: The goal of this study was to examine the causes and risk factors (RF) for renal GL in the era since the widespread adoption of single antigen bead testing for donor and compare to prior studies based on surveillance biopsies (El Zogby et al AJT 2109;9:527).
*Methods: We retrospectively determined the causes of GL in two transplant (Tx) programs in conventional Kidney Transplant (KTx) performed from 1/1/2006 to 10/1/2018. Patient data and RF were abstracted and the diagnosis(Dx) of GL was determined by two Tx nephrologists that independently reviewed the charts, with disagreements in the Dx arbitrated by other two Tx nephrologists. Early technical losses were excluded. To assess RF for GL we also used a Nested-Case Control model (matched in 2:1 ratio, by age, Tx year, type of donor, and Tx center).
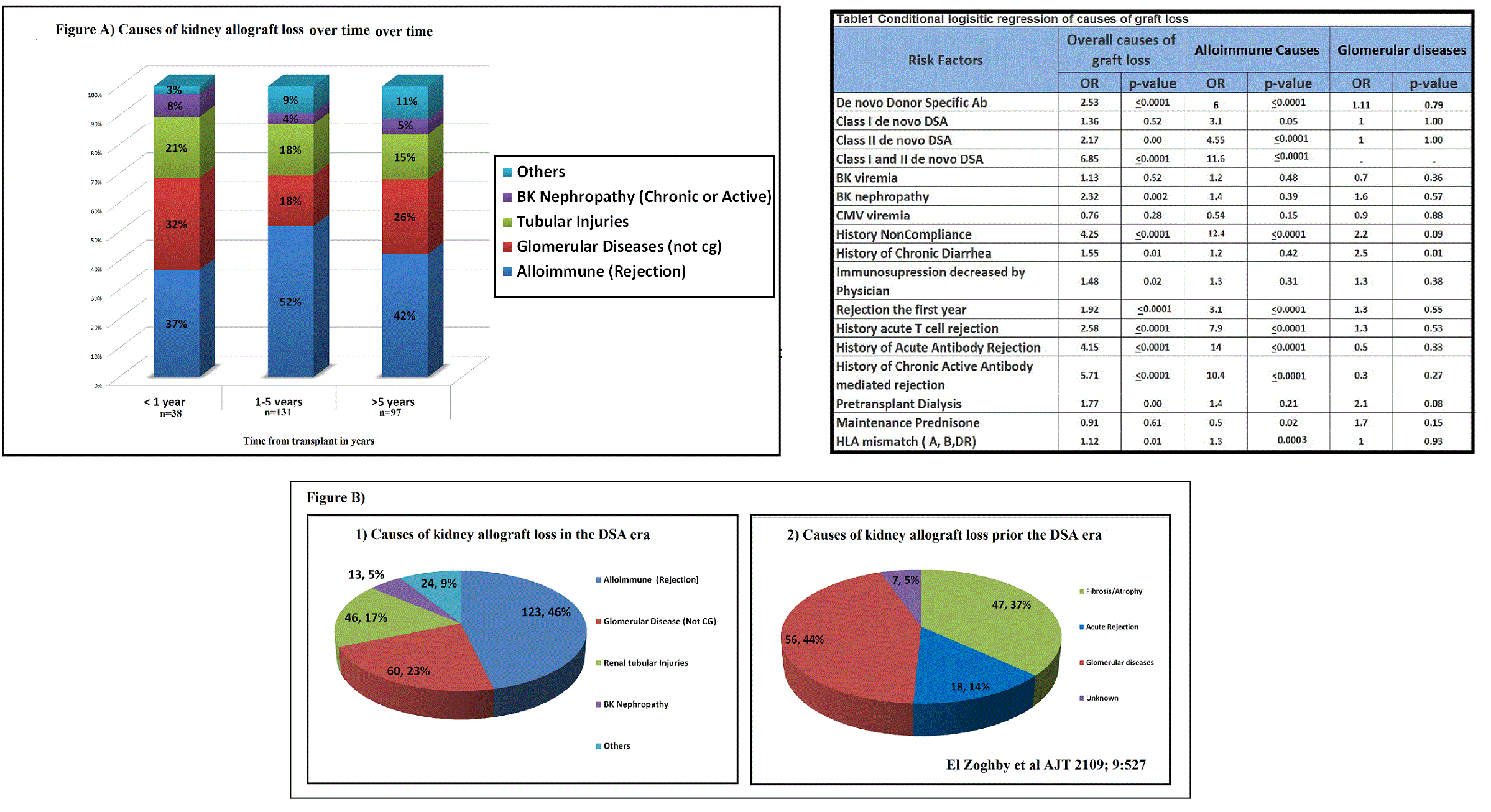
*Results: There were total of 4164 adult solitary KTx. Deaths with functioning graft occurred in 404 (9.7%) including: malignancy 23%, infection 21%, cardiac 12%, other 11% and unknown 33%. Death-censored GL occurred in 266 (6.4%) including 38 in the first year, 131 between 1-5 years and 97 >5 years (Figure A). Causes of GL were similar over time suggesting that length of follow-up likely did not affect our assessment of overall GL. Overall death-censored graft loss with up to 10 years follow-up included: alloimmune 46%, non-alloimmune glomerular diseases 22.6%, renal tubular damages 17% (acute kidney injury, recurrent hypovolemia, urinary tract infections, etc.); BK nephropathy 13% and others 9%. Compared to studies prior to the widespread use of single antigen DSA testing, the current cohort had higher rates of GL attributed to alloimmunity , fewer cases of glomerular disease and even fewer cases attributed solely to fibrosis and atrophy (FigureB). RF for GL were similar to the causes (Table1) were: Hx of chronic active antibody mediated rejection OR=5.7 (p<0.001), noncompliance OR=4.3(p<0.001), Hx acute antibody mediated rejection OR=4.2 (p< 0.001), Hx of acute T cell mediated rejection OR=2.6 (p< 0.001), de novo DSA OR=2.5 (p<0.001), Class II DSA OR=2.2 (p<0.001), BK nephropathy OR=2.3(p=0.002) and rejection the first year OR=1.9(p=0.001).
*Conclusions: In the current era of DSA testing, alloimmunity with or without non-adherence is the most common cause of GL being evenly distributed over the first 10 years after KTX. However, glomerular diseases, BK virus and tubular damage account more than 50% of GL and thus also should be part of efforts to improve long-term graft survival.
To cite this abstract in AMA style:
Merzkani M, Benavides X, D'Costa M, Smith B, Park W, Rule A, Chakkera H, Reddy K, Alexander M, Amer H, Ters MEl, Schinstock C, Heilman R, Bentall A, Stegall M. Causes of Kidney Allograft Loss (GL) in the Current Era of Donor-Specific Alloantibody (DSA) Testing [abstract]. Am J Transplant. 2020; 20 (suppl 3). https://atcmeetingabstracts.com/abstract/causes-of-kidney-allograft-loss-gl-in-the-current-era-of-donor-specific-alloantibody-dsa-testing/. Accessed May 17, 2026.« Back to 2020 American Transplant Congress