Accumulation of Highly Sensitized Patients in a KPD Registry.
University of Toledo, Toledo, OH.
Meeting: 2016 American Transplant Congress
Abstract number: 425
Keywords: Kidney transplantation, Sensitization
Session Information
Session Name: Concurrent Session: Kidney Paired Exchange: Outcomes and Issues
Session Type: Concurrent Session
Date: Tuesday, June 14, 2016
Session Time: 2:30pm-4:00pm
 Presentation Time: 3:42pm-3:54pm
Presentation Time: 3:42pm-3:54pm
Location: Ballroom C
Objectives: We analyzed sensitization against HLA among patients in a kidney paired donation (KPD) registry. In particular, three groups of patients were included: 1) all KPD registered patients between 2010 and 2015 (1032 patients); 2) patients on the active match run list in 2015 (157 patients); and 3) all transplanted recipients between 2010 and 2015 (219 patients). Methods/Results: Sensitization of patients was reported by the transplant centers as calculated panel reactive antibody (PRA) and a list of unacceptable antigens. Among all registered patients, 30% were non-sensitized (PRA 0%), 29% had a PRA 1-79%, 41% were highly sensitized (PRA 80-100%) and 25% of patients had PRA 95-100% [Figure 1; top]. Level of sensitization of patients on the active list was higher, as 47% had a PRA 80-100% and 35% had PRA over 95%. The sensitization was different among transplanted patients; 47% were mildly (PRA 1-79%) and only 24% were highly (PRA=80-100%) sensitized; 12% had a PRA over 95%. We analyzed patterns of sensitization against HLA-A, B, C, DR, DQ and DP antigens across different PRA levels [Figure 1; bottom]. Perhaps most strikingly, nearly 50% of highly sensitized active match run patients are sensitized to DPB antigens and nearly 30% to DQA antigens. Finally, waiting times were calculated based on registration and transplantation dates as reported by the transplant centers. Notably, the level of sensitization affected the waiting time: non-sensitized recipients waited an average of 199 days; those with a PRA of 1-79% waited 231 days; those with a PRA of 80-100% waited 393 days; and those with a PRA of 95-100% waited 524 days. Conclusions: Although KPD registries were designed to accommodate highly sensitized patients, these patients accumulate on the waiting list. An increasing number of patients are sensitized to DPB and DQA; however, this is not reflected in their UNOS PRA and can result in false negative virtual crossmatches. Therefore, all HLA genes should be used for matching, especially in sensitized patients. As such, we plan to establish an acceptable mismatch program for highly sensitized patients to increase their chances of getting a kidney transplant. 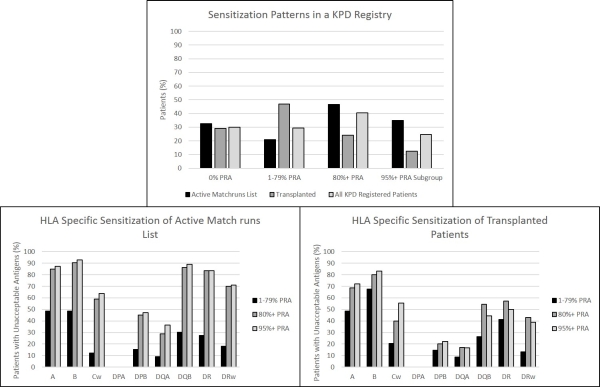
CITATION INFORMATION: Stepkowski S, Mierzejewska B, Bekbolsynow D, Rees M. Accumulation of Highly Sensitized Patients in a KPD Registry. Am J Transplant. 2016;16 (suppl 3).
To cite this abstract in AMA style:
Stepkowski S, Mierzejewska B, Bekbolsynow D, Rees M. Accumulation of Highly Sensitized Patients in a KPD Registry. [abstract]. Am J Transplant. 2016; 16 (suppl 3). https://atcmeetingabstracts.com/abstract/accumulation-of-highly-sensitized-patients-in-a-kpd-registry/. Accessed May 22, 2026.« Back to 2016 American Transplant Congress
