A Mechanistic Evaluation to Guide the Optimal Immunosuppression Adjustment Strategy in Transplant Patients with COVID-19
UHN, Toronto, ON, Canada
Meeting: 2021 American Transplant Congress
Abstract number: LB 2
Keywords: COVID-19, Immunosuppression, T cell activation, T cells
Topic: Clinical Science » Infectious Disease » COVID-19
Session Information
Session Name: Late-Breaking: COVID-19
Session Type: Rapid Fire Oral Abstract
Date: Monday, June 7, 2021
Session Time: 4:30pm-5:30pm
 Presentation Time: 4:35pm-4:40pm
Presentation Time: 4:35pm-4:40pm
Location: Virtual
*Purpose: The optimal management of immunosuppression in transplant patients infected with COVID-19 is unknown. Reduction in calcineurin inhibitors or antimetabolite doses is often performed in order to enhance immune responses, but there are minimal data to guide decisions. We performed an in vitro study to determine the effect of individual immunosuppressive agents and doses on SARS-CoV-2 specific T-cell cytokine expression.
*Methods: Peripheral blood mononuclear cells (PBMCs) were isolated from nine non-immunosuppressed patients diagnosed with COVID-19 at least 14 days prior. Cells were pre-incubated for four hours with clinically relevant, differing concentrations of immunosuppressive drugs (tacrolimus (TAC), mycophenolate (MPA), sirolimus, prednisone). PBMCs were then stimulated with SARS-CoV-2 spike and nucleoprotein peptide pools for 24 hours with appropriate positive and negative controls. Supernatants collected were analyzed by a 14-plex high sensitivity T-cell cytokine array (Eve Technologies).
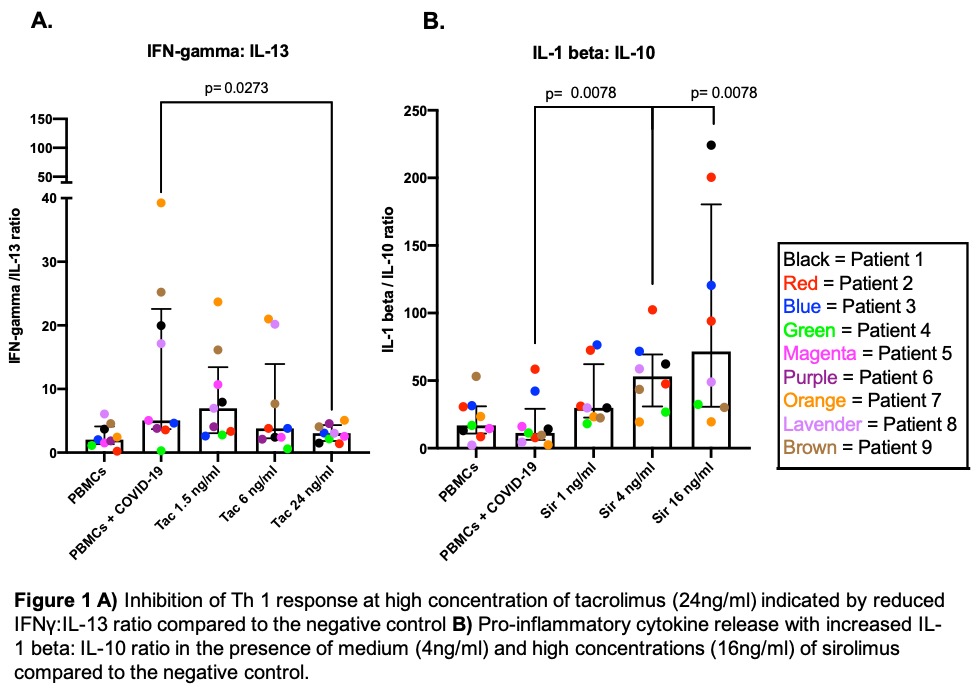
*Results: PBMCs stimulation with SARS-CoV-2 peptides resulted in broad cytokine responses. In the presence of TAC at medium (6ng/ml) and high concentrations (24ng/ml) (both are commonly achieved trough/peak clinical concentrations respectively), there were significantly reduced levels of IL-2 (p=0.0078 for both), and at high concentrations, lower amounts of IFN-γ (p= 0.0391) in response to peptide stimulation. TAC (24ng/ml) also resulted in a skewing of the response from a TH1 to a TH2 phenotype as indicated by lower IFN-γ: IL-13 ratio (p=0.0273), and IFN-γ: IL-4 ratio (p=0.0234). In contrast, differing clinically relevant concentrations of MPA and prednisone did not appear to influence the cytokine response post-peptide stimulation. Interestingly, Sirolimus at medium (4ng/ml) and high (16ng/ml) concentrations was found to be significantly associated with pro-inflammatory cytokine release in response to SARS-CoV-2 peptides; TNF-α (p=0.0078 for both), IL-6 (p=0.0234 for both) and IL-1β (p=0.0156 and p=0.0078, respectively). When expressed as a pro- vs. anti-inflammatory ratio (with IL-10 as the anti-inflammatory cytokine), this finding remained consistent.
*Conclusions: These in-vitro results could help guide clinical decisions. Greater concentrations of TAC led to an inhibition of Th1 responses, whereas sirolimus led to an unexpected proinflammatory response, and MPA was neutral. This suggests that for transplant patients with COVID-19, a reduction of TAC may be of greater benefit than MPA. For those on sirolimus, reduction should be considered if evidence of an inflammatory phase.
To cite this abstract in AMA style:
Hall V, Ferreira V, Kumar D, Humar A. A Mechanistic Evaluation to Guide the Optimal Immunosuppression Adjustment Strategy in Transplant Patients with COVID-19 [abstract]. Am J Transplant. 2021; 21 (suppl 3). https://atcmeetingabstracts.com/abstract/a-mechanistic-evaluation-to-guide-the-optimal-immunosuppression-adjustment-strategy-in-transplant-patients-with-covid-19/. Accessed April 4, 2026.« Back to 2021 American Transplant Congress