Renal Allograft Survival of HLA-Identical Living Donors (ID-LDRT) and 6-HLA Matched Cadaveric Donors (6M-CRT) Compared with 5 HLA-Matched Controls
Division of Transplant Surgery, Starzl Transplantation Institute, University of Pittsburgh Medical Center, Pittsburgh, PA
Division of Transplant Nephrology, Starzl Transplantation Institute, University of Pittsburgh Medical Center, Pittsburgh, PA
Meeting: 2013 American Transplant Congress
Abstract number: C1230
Introduction:
ID-LDRT and 6M-CRT HLA recipients are thought to enjoy superior outcomes compared with those with 1 HLA lesser matching (5 HLA matched controls; 5M). We studied the outcome of each group, and indirectly explored the relative importance of minor-HLA and non-HLA matching.
Methodology:
ID-LDRT (n=62) and 6M-CRT (n=94) recipients at our center between 1988-2012 were identified. Controls were those with 5 HLA match within each group (n=42, and n=131, respectively), and matched for gender, age, and cold ischemia time (CIT). We compared actuarial renal allograft and patient survival using Kaplan-Meier log-rank test between ID-LDRT and 5M-LDRT as well as 6M-CRT and 5M-CRT. Significance was set at p<0.05.
Results:
There were no differences between the groups on patient age, sex, ethnicity, or CIT. The median graft survival (Figure 1) was superior in the ID-LDRT (16 years, p=0.008).
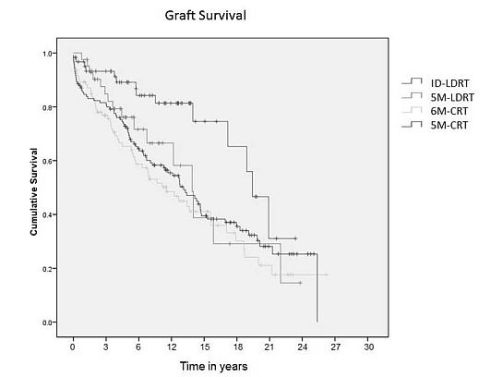
Graft survival was not significantly different in the other 3 groups; 5M-LDRT (10.9 years), 6M-CRT (8.5 years), and 5M-CRT (10.1 years). There was no significant difference in patient survival.
Conclusion:
In this analysis, there was no incremental graft survival benefit of 6M CRT over the next-best category, the 5M-CRT. ID-LDRT (siblings) enjoyed a 5 year median graft survival increase over their 1 HLA mismatched controls. Our data suggests that non-HLA and minor HLA antigens impact graft loss. These results need to be confirmed by analyzing national data, and correlated to immunosuppression exposure.
To cite this abstract in AMA style:
Gunabushanam V, Nusrat R, Lam H, Sood P, Hariharan S, Donaldson J, Humar A, Wijkstrom M. Renal Allograft Survival of HLA-Identical Living Donors (ID-LDRT) and 6-HLA Matched Cadaveric Donors (6M-CRT) Compared with 5 HLA-Matched Controls [abstract]. Am J Transplant. 2013; 13 (suppl 5). https://atcmeetingabstracts.com/abstract/renal-allograft-survival-of-hla-identical-living-donors-id-ldrt-and-6-hla-matched-cadaveric-donors-6m-crt-compared-with-5-hla-matched-controls/. Accessed May 22, 2026.« Back to 2013 American Transplant Congress
