Opioid Use Prior to Liver Transplant is Associated with Increased Risk of Death after Transplant
University of California, San Francisco, San Francisco, CA
Meeting: 2020 American Transplant Congress
Abstract number: 477
Session Information
Session Name: Liver: Recipient Selection
Session Type: Oral Abstract Session
Date: Saturday, May 30, 2020
Session Time: 3:15pm-4:45pm
 Presentation Time: 3:15pm-3:27pm
Presentation Time: 3:15pm-3:27pm
Location: Virtual
*Purpose: The impact of the opioid epidemic on liver transplant (LT) candidates and recipients has not been widely studied, but pre-LT opioid use in LT candidates is estimated at 25-30%. Furthermore, for opioid naïve patients, any surgery introduces a 6-10% risk of developing chronic opioid use post-operatively. Therefore, the purpose of this study was to describe opioid use in LT recipients before and after transplant and to determine whether prior opioid use impacted post-LT opioid use, graft survival, or patient survival.
*Methods: A retrospective review of all adult LT recipients at our institution between 2012-2019 was performed. Patients were excluded if they received a multiorgan transplant or were re-transplant recipients. Descriptive statistics were computed, stratified according to opioid use prior to transplant, and compared using Mann Whitney and Chi squared tests (significance p<0.05). UV and MV regression models were used to determine predictors of oral morphine equivalents (OME) at discharge (DC), days of opioids prescribed, and post-LT refills (p<0.1 for inclusion in MV model). Graft and patient survival were evaluated using Kaplan Meier analysis.
*Results: 762 patients underwent LT during the study period, of whom 126 (16.5%) had a history of prior opioid use. Compared with patients with no prior opioid use, there were no significant differences in age (56.5 prior opioid vs. 56.2), gender (31% vs. 34.3% female), race (36.5% vs. 43.4% Caucasian), etiology of liver disease (34.9% vs. 30.2% HCV), history of depression (6.3% vs. 7.9%), donor type (84.1% vs. 83.2% deceased donor), or match MELD (31.8 vs. 31.2). Patients with prior opioid use had higher OME during the day prior to DC (55.8 vs. 32.9, p=0.03), greater total OME prescribed at DC (456 vs. 317, p=0.01), and more refills at 30-60 days after LT (29.4% vs. 19.7%, p=0.02). At 60-90 days post-transplant, 10.7% of opioid naïve patients and 13.5% of patients with prior opioid use still required refills.
In MV linear regression, longer post-operative length of stay, prior opioid status, and a greater number of OME on the day prior to DC were associated with increased maximum OME at DC and total OME at DC.
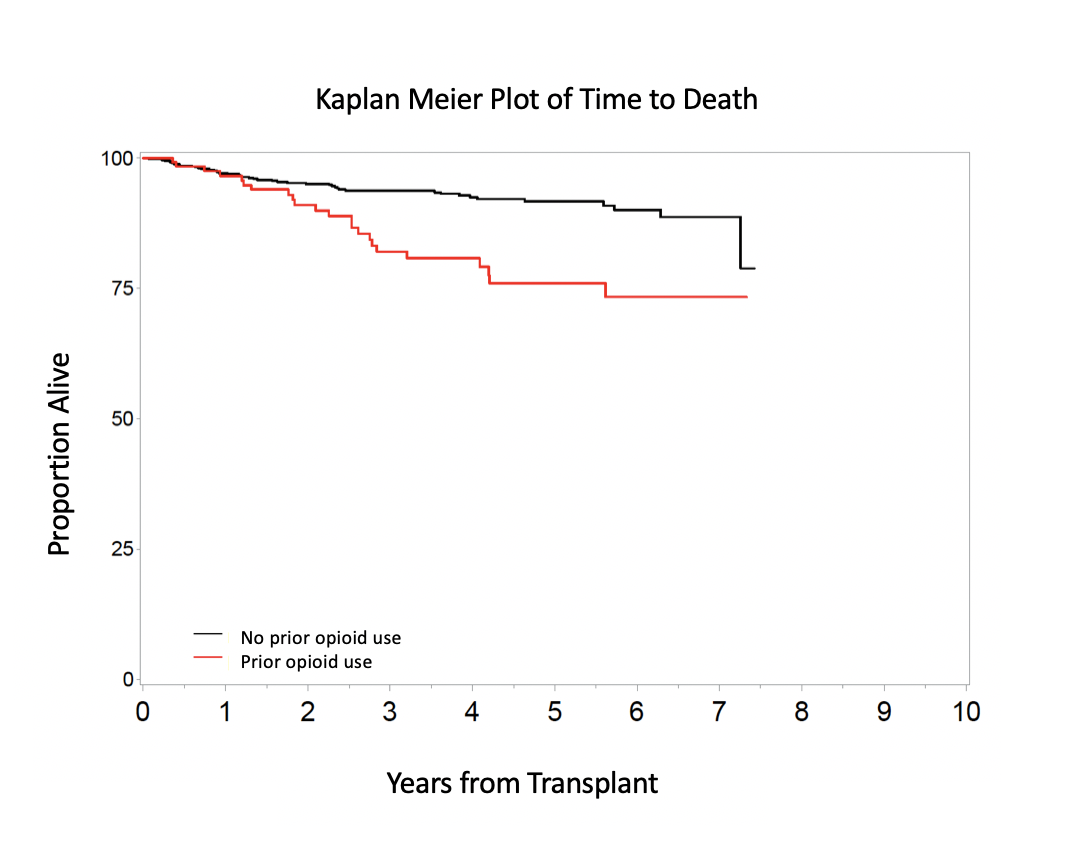
There was no difference in graft survival among the two groups, but patient survival was significantly worse in patients with an opioid history compared with those who were opioid naïve (Figure, p<0.001).
*Conclusions: At 60-90 days after LT, more than 10% of LT recipients require ongoing opioid refills. Opioid use prior to LT is associated with increased risk of death after LT.
To cite this abstract in AMA style:
Braun HJ, Schwab MP, Jin C, Amara D, Grace T, Croci R, Freise CE, Roberts JP, Hirose R, Ascher NL. Opioid Use Prior to Liver Transplant is Associated with Increased Risk of Death after Transplant [abstract]. Am J Transplant. 2020; 20 (suppl 3). https://atcmeetingabstracts.com/abstract/opioid-use-prior-to-liver-transplant-is-associated-with-increased-risk-of-death-after-transplant/. Accessed July 12, 2025.« Back to 2020 American Transplant Congress