Living Donor Rates Vary Greatly Among Organ Procurement Organizations in the United States.
Medicine, University of Virginia, Charlottesville, VA.
Meeting: 2016 American Transplant Congress
Abstract number: A140
Keywords: Donation, Kidney transplantation
Session Information
Session Name: Poster Session A: Kidney Donor Outcomes
Session Type: Poster Session
Date: Saturday, June 11, 2016
Session Time: 5:30pm-7:30pm
 Presentation Time: 5:30pm-7:30pm
Presentation Time: 5:30pm-7:30pm
Location: Halls C&D
Introduction: Living donor kidney transplant remains the optimal renal replacement therapy in ESRD. Despite known benefits of living donation (LD), rates vary significantly among organ procurement organizations (OPOs). We sought to understand the regional differences in LD rates.
Methods: Using the SRTR, all adult candidates listed for kidney or kidney pancreas transplant between 2001 and 2010 were identified (N=268,179). Univariate analysis was performed to show candidate LD rates by OPO of first listing. Further logistic regression analyses were performed looking at multiple candidate covariates including age, race/ethnicity, gender, etiology of ESRD, ABO type, initial listing status (active or inactive), primary insurance, educational attainment, kidney pancreas listing, and event listing (primary transplant or re-transplant).
Results: Our analyses showed large differences in LD rates by OPO, ranging from 3.7% to 42% of candidates receiving a living donor transplant within 2.5 years of listing.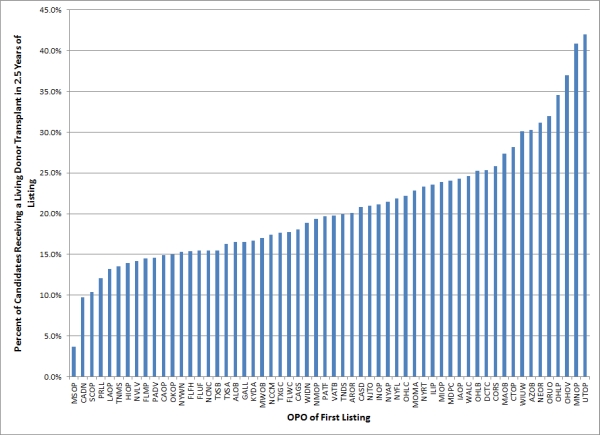 Rates of LD varied by a factor of over 9, even adjusting for candidate factors known to be influence LD.
Rates of LD varied by a factor of over 9, even adjusting for candidate factors known to be influence LD.
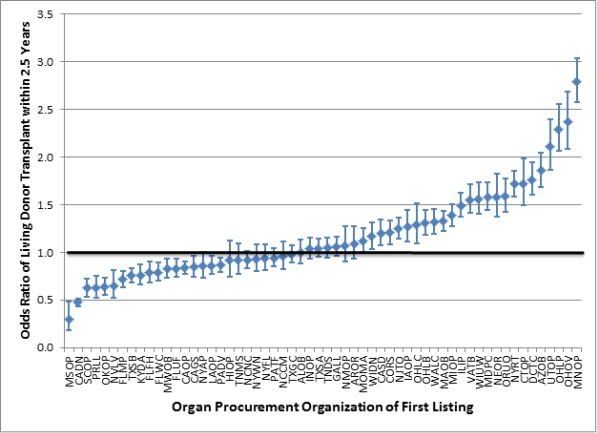
Discussion: Rates of LD vary greatly by OPO. Increased access to LD can decrease pressure on the deceased donor pool. A better understanding of the factors driving regional differences in LD may help the transplant community address barriers to donation and improve access to living donor kidney transplant in the United States.
CITATION INFORMATION: Keith D, Nishio Lucar A, Vranic G. Living Donor Rates Vary Greatly Among Organ Procurement Organizations in the United States. Am J Transplant. 2016;16 (suppl 3).
To cite this abstract in AMA style:
Keith D, Lucar ANishio, Vranic G. Living Donor Rates Vary Greatly Among Organ Procurement Organizations in the United States. [abstract]. Am J Transplant. 2016; 16 (suppl 3). https://atcmeetingabstracts.com/abstract/living-donor-rates-vary-greatly-among-organ-procurement-organizations-in-the-united-states/. Accessed May 24, 2026.« Back to 2016 American Transplant Congress
