Ethical and Financial Consequences of Incidental Radiological Findings During Living Kidney Donor Evaluation
University of Texas Medical Branch, Galveston, TX
Meeting: 2020 American Transplant Congress
Abstract number: B-032
Keywords: Donation, Ethics, Kidney, Radiologic assessment
Session Information
Session Name: Poster Session B: Kidney Living Donor: Other
Session Type: Poster Session
Date: Saturday, May 30, 2020
Session Time: 3:15pm-4:00pm
 Presentation Time: 3:30pm-4:00pm
Presentation Time: 3:30pm-4:00pm
Location: Virtual
*Purpose: Living kidney donation (LKD) provides a unique situation in that diagnostic studies are ordered on a presumably healthy individual. Literature has shown that preoperative tests often detect clinically significant findings, but whether or not these ultimately benefit or cause detriment to patients is still up for debate. Further, these tests are not without cost in both a monetary and emotional sense. The purpose of this study is to highlight and explore the ethical and financial consequences of incidental radiological findings during evaluation for LKD at our institution.
*Methods: A retrospective review of referrals for LKD that progressed to evaluation between February 2014 and October 2019 was performed. Demographic data and radiological findings, which included abdominal ultrasonography (US), computed tomography (CT) of the chest and/or abdomen/pelvis, and chest roentgenography (CXR), were obtained from medical records.
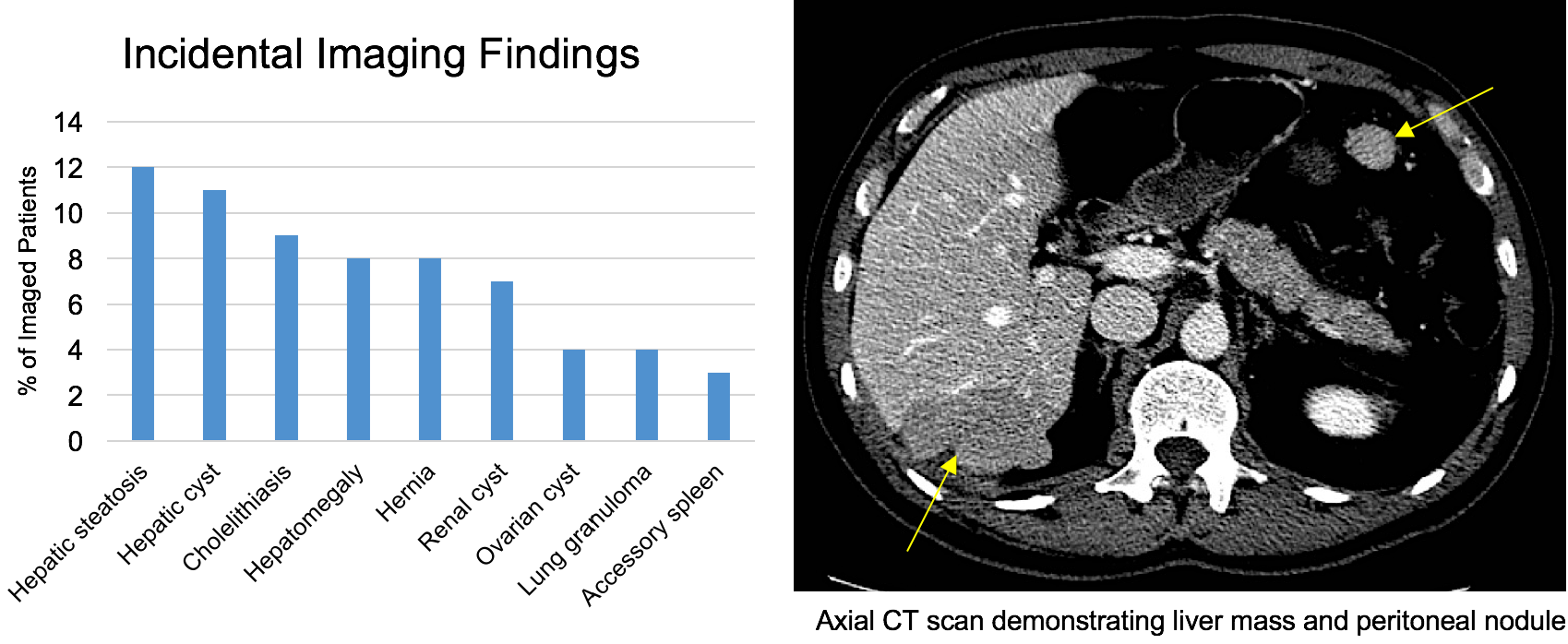
*Results: One hundred and fifteen LKD evaluations were reviewed, of which 89 potential donors were imaged. Notable incidental findings were present in 1% of CXR, 36% of US, and 77% of CT. The most common incidental findings were hepatic steatosis and hepatic cysts. Ultimately, 28 (24%) evaluations resulted in a transplant. One patient had imaging concerning for a malignancy, and his case highlights the ethical and financial dilemma of an incidental finding. This potential donor had a suspicious liver mass and peritoneal nodules. He underwent biopsy of the mass, which revealed normal hepatocytes. This was suspected to be sampling error, but further investigation was terminated by the patient as he was required to pay out-of-pocket toward his insurance plan deductible. Billing to the global kidney acquisition charge ceased when the investigation of the incidental finding began. For this individual, his preoperative evaluation not only failed to result in a kidney donation but also caused him financial strain and worry.
*Conclusions: In conclusion, although the majority of living kidney donor evaluations do not progress to organ donation, much clinical information is obtained during the evaluation process, and the ethical guidelines regarding the disclosure obligations of these data are not well defined. Additionally, when the personal sacrifice of the living donor expands during the LKD evaluation process without resulting in a transplant, what obligation does the program have to see that the principles of beneficence and non-maleficence are best served?
To cite this abstract in AMA style:
Mao R, Kulkarni R, Duran C, Stevenson-Lerner H, Mujtaba M, Fair J, Kueht M. Ethical and Financial Consequences of Incidental Radiological Findings During Living Kidney Donor Evaluation [abstract]. Am J Transplant. 2020; 20 (suppl 3). https://atcmeetingabstracts.com/abstract/ethical-and-financial-consequences-of-incidental-radiological-findings-during-living-kidney-donor-evaluation/. Accessed May 16, 2026.« Back to 2020 American Transplant Congress