Diminishing Scientific Registry of Transplant Recipients Risk-Adjusted Mortality: Reaction to Flagging, Artifact of Modeling, or Both?
1Division of Nephrology, Hypertension, and Renal Transplantation, University of Florida, Gainesville, FL, 2Shands Transplant Center, University of Florida, UF Health Shands, Gainesville, FL, 3Department of Surgery, University of Florida, Gainesville, FL
Meeting: 2019 American Transplant Congress
Abstract number: 282
Keywords: Mortality, Outcome, Prediction models, Survival
Session Information
Session Name: Concurrent Session: Quality Assurance Process Improvement & Regulatory Issues I
Session Type: Concurrent Session
Date: Monday, June 3, 2019
Session Time: 2:30pm-4:00pm
 Presentation Time: 2:42pm-2:54pm
Presentation Time: 2:42pm-2:54pm
Location: Room 210
*Purpose: To examine longitudinal trends in SRTR risk-adjusted patient and graft survival rates.
*Methods: Current, and archived versions of The Scientific Registry of Transplant Recipients (SRTR) “National Center-Level Summary Data by Organ” were downloaded from the SRTR Website and imported into statistical programming software. Individual transplant centers, for each organ, were selected for analysis based on a specified volume of transplants maintained across the 13 Program Specific Reports (PSR) represented (2012 – 2018). Risk-adjusted mortality for each center was then calculated as [100 – risk-adjusted survival]. Data was then evaluated with a linear mixed effect model to account for center-to-center variability and within-center correlation.
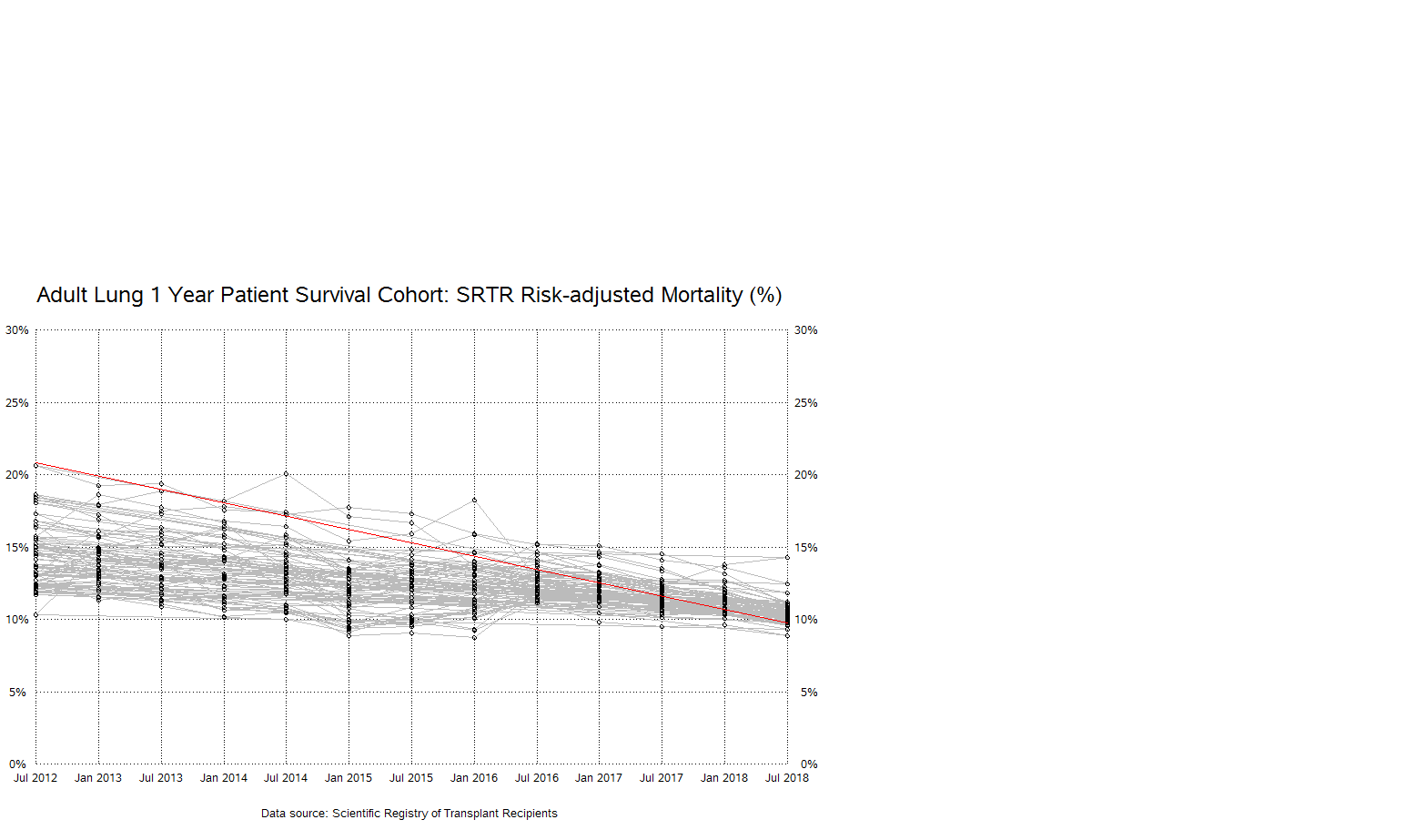
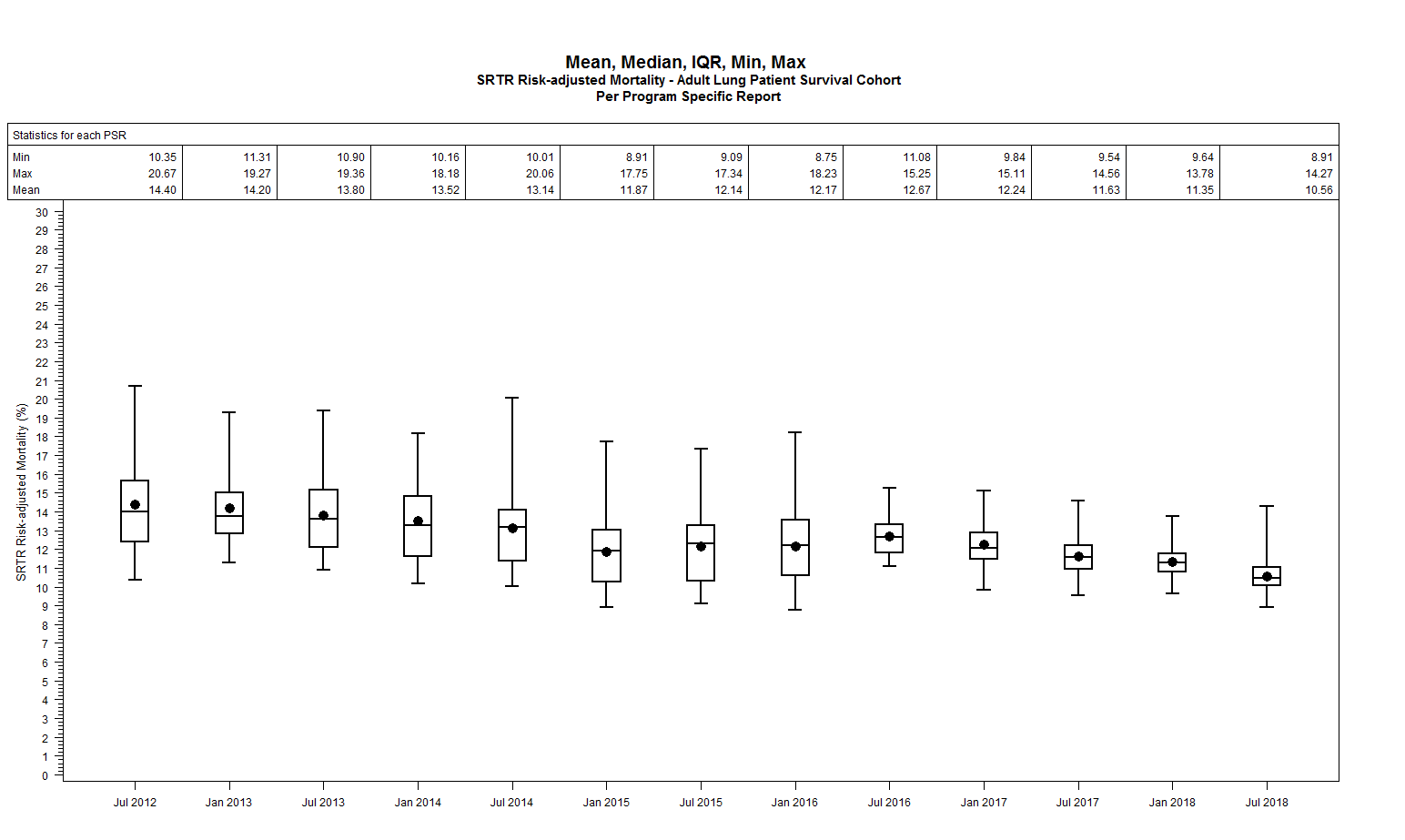
*Results: For each different patient and graft survival cohort examined (adult heart, kidney, liver, and lung), the expected mortality decreased significantly (p < 0.001) over time. Adult lung patient survival is used as an example in the figures seen below. $$20181130 - GE 20 TXs Adult Lung PS Spag with Trend.png_ $$20181130 - GE 20 Adult Lung PS Box Chart.png_
*Conclusions: A significant downward trend, accompanied by decreased variability, in expected probability (adjusted for patient and donor characteristics) of patient or graft survival at 1 year is observed for all organs considered in this analysis. Across the 13 PSRs analyzed there clearly has been a ‘regression to the mean’ throughout the entirety of the solid organ transplant effort in the United States. It is plausible that the observed effect is due to a reaction by centers to increasing outcomes oversight and regulation by the Organ Procurement and Transplantation Network/Membership and Professional Standards Committee, and the Centers for Medicare and Medicaid Services. Numerous publications over the years rally the concern that very low failure estimates may be leading to the continued high risk of donated allograft non-use and more careful selection of riskier candidates.* It has been argued that traditional outcome regulation, with its near singular reliance on SRTR expected patient and graft survival values, has resulted in perhaps ‘too good’ of outcomes when considering the larger potential donor and recipient pools that are likely being underserved by programs due to regulatory concerns. Only changing the harshness of the expectations and/or regulatory oversight, and also taking into account risk factors currently not considered, will allow centers to use more of the currently discarded donated organs and consider riskier candidates. *i.e. Schold et al. writing in the American Journal of Transplantation showed that kidney centers with statistically significant lower than expected 1-year graft or patient survival subsequently decreased transplant volume, and “had a reduction in use of donors with extended cold ischemia time.”1
1. Schold JD, Buccini LD, Srinivas TR, et al. The association of center performance evaluations and kidney transplant volume in the United States. Am J Transplant. 2013 Jan;13(1):67-75. Available from: https://onlinelibrary.wiley.com/doi/full/10.1111/j.1600-6143.2012.04345.x
To cite this abstract in AMA style:
Gregg JA, Womer KL, Santos A, Moore SJ, Andreoni KA. Diminishing Scientific Registry of Transplant Recipients Risk-Adjusted Mortality: Reaction to Flagging, Artifact of Modeling, or Both? [abstract]. Am J Transplant. 2019; 19 (suppl 3). https://atcmeetingabstracts.com/abstract/diminishing-scientific-registry-of-transplant-recipients-risk-adjusted-mortality-reaction-to-flagging-artifact-of-modeling-or-both/. Accessed May 23, 2026.« Back to 2019 American Transplant Congress