Development and Prospect of Donation after Cardiac Death in China
Department of General Surgery and Organ Transplantation, The First Hospital of China Medical University, Shenyang, Liaoning, China
Meeting: 2013 American Transplant Congress
Abstract number: C1255
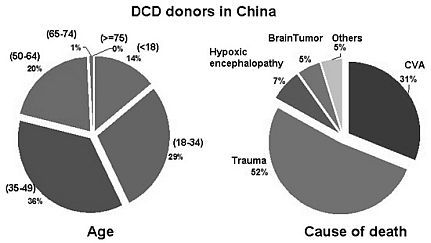
From March 2010, a pilot program of organ donation in human has been implemented by China Red Cross Society and the Ministry of Health (MOH). Three categories of deceased donors were defined by Organ Transplantation Committee, including (I) donation after brain death (DBD), (II) donation after cardiac death (DCD), and (III) donation after brain death and cardiac death (DBCD). Meanwhile, a nation-wide project in DCD led by our group was funded by an ad hoc grant of MOH, collaborating with 20 other transplant centers. We also developed an internet-based registry of DCD in China for large scale statistical analysis. From March 2010 to November 2012, centers in our project have performed 300 cases of DCD, accounting 62.22% of the numbers in China. The percentages of donors in each category are 8.2% (I), 39% (II), and 52.8% (III) respectively. The average age of donors is 35.95, with 65% of donors aged between 18 and 49, which is higher than that (55%) in the united network for organ sharing. Differences between the two groups were found in the causes of death, with more trauma in China (52% vs 32%), less hypoxic encephalopathy (7% vs 30%), and an equivalent cerebrovascular accident (31% vs 34.6%). 621 organs were procured (47.77% of China), leading to 384 kidney, 234 liver, and 3 pancreas transplantations. The average warm ischemic times in liver and kidney are around 6 and 7 minutes, with the cold ischemic times as 7.5 and 5.2 hours. Post-transplantation complications were detected in 24 kidney recipients, including 19 delayed graft function, 3 bleeding or thrombosis, and 2 primary non function. In contrast, 23 liver recipients developed complications, including 6 primary non function, 5 biliary complications, 4 infection, 4 vascular complications, and 4 tumor recurrence. Extracorporeal membrane oxygenation saved 30% of low-quality organs. In addition, 39 Kidneys treated with hypothermic mechanical perfusion showed a remarkable improvement in graft function (P<0.05), indicated by the initial time of urination, peri-operative urine volume, and the reduction of blood creatinine level. These results provided important guidance for the clinical practice of DCD in China.
To cite this abstract in AMA style:
Liu Y. Development and Prospect of Donation after Cardiac Death in China [abstract]. Am J Transplant. 2013; 13 (suppl 5). https://atcmeetingabstracts.com/abstract/development-and-prospect-of-donation-after-cardiac-death-in-china/. Accessed May 24, 2026.« Back to 2013 American Transplant Congress
