Characterization Of Microscopic Hematuria Following Renal Transplant
1Department of Urology, Kidney and Pancreas Transplant Programs, UCLA, Los Angeles, CA, 2Division of Nephrology, Kidney and Pancreas Programs, UCLA, Los Angeles, CA
Meeting: 2019 American Transplant Congress
Abstract number: C49
Keywords: Kidney, Post-transplant malignancy, Resource utilization, Urinalysis
Session Information
Session Name: Poster Session C: Kidney Complications: Late Graft Failure
Session Type: Poster Session
Date: Monday, June 3, 2019
Session Time: 6:00pm-7:00pm
 Presentation Time: 6:00pm-7:00pm
Presentation Time: 6:00pm-7:00pm
Location: Hall C & D
*Purpose: The American Urological Association (AUA) recommends a CT Urography and cystoscopy for the evaluation of a single episode of microscopic hematuria (MH) in the absence of an obvious etiology. Renal transplant recipients (RTR) frequently have postoperative MH, possibly attributable to surgery, however no data exists regarding the prevalence and duration. The characterization of MH following renal transplant (RT) may portend tailored decision-making strategies for malignancy evaluation purposes in this population and limit costly and invasive diagnostics.
*Methods: Between 2006 and 2016 over 3,200 patients underwent RT at our institution for whom post-operative microscopic urine analyses (UA) were analyzed. Presence of MH was assessed at postoperative months 1, 2, 3, 6, 9, and 12. Stents are routinely placed in all patients and removed at 1 month. Microscopic hematuria was defined as ≥ 11 RBCs/HPF based on assay sensitivity. Urine culture was deemed positive if ≥ 100k bacteria CFU/mL, BK viremia (BKV) was defined by ≥ 1k copies/mL via PCR, and percutaneous allograft biopsy was deemed recent if within 30 days before MH episode. The quantitative trend of MH among 548 RTRs who had UA results available at all time intervals was assessed. The overall prevalence of MH among all RTRs with UA results at each specific time interval was assessed.
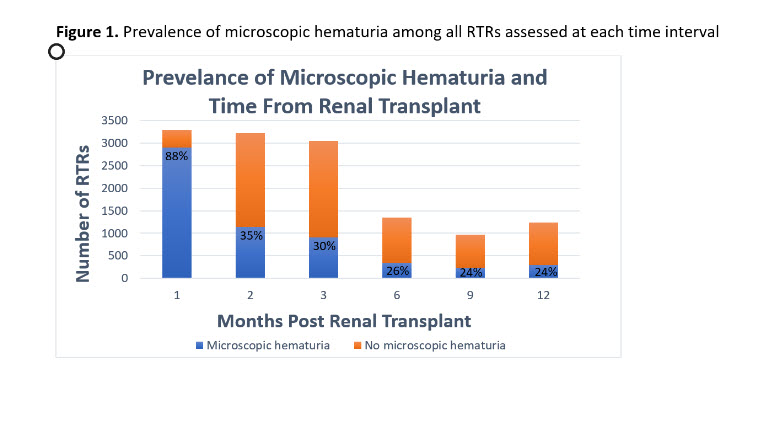
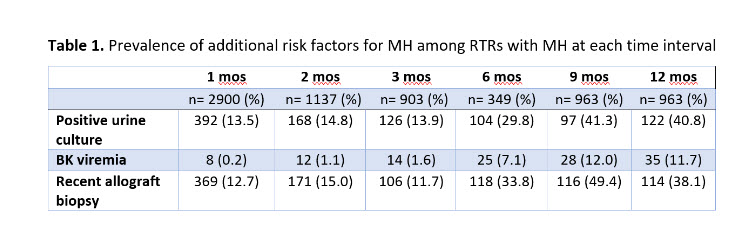
*Results: The prevalence of MH was 88% at postoperative month 1, 35% at 2 months, 30% at 3 months, 26 % at 6 months, 24% at 9 months, and 24 % at 1 year (Figure 1). Thirty-five percent of RTRs experienced 3 or more episodes of MH within postoperative year 1 in an intermittent pattern. Over one third of RTRs with MH were found to have a positive urine culture and/or recent allograft biopsy at months 6,9, and 12 (Table 1).
*Conclusions: This is the first study to characterize MH among RTRs. Microscopic hematuria in RTRs is common in the first 1 to 2 months postoperatively and is likely related to surgical trauma. However, 24% to 30% of patients will continue to have intermittent MH which is significantly greater than the general population and is less likely due to malignancy given the frequency of unique transplant sequala. These findings highlight the need for additional MH associated malignancy risk adjustment models in RTRs.
To cite this abstract in AMA style:
McDonald ML, Duong TN, Datta N, Gritsch HA, Bunnapradist S. Characterization Of Microscopic Hematuria Following Renal Transplant [abstract]. Am J Transplant. 2019; 19 (suppl 3). https://atcmeetingabstracts.com/abstract/characterization-of-microscopic-hematuria-following-renal-transplant/. Accessed May 21, 2026.« Back to 2019 American Transplant Congress