Belatacept versus Tacrolimus Combined with Antithymocyte Globulin in Kidney Transplantation
1Swedish Medical Center, Seattle, WA, 2SUNY, Brooklyn, NY, 3Permanente Medical Group, Oakland, CA
Meeting: 2020 American Transplant Congress
Abstract number: 110
Keywords: Co-stimulation, Immunosuppression, Infection, Outcome
Session Information
Session Name: Novel Immunosuppression: Belatacept
Session Type: Oral Abstract Session
Date: Saturday, May 30, 2020
Session Time: 3:15pm-4:45pm
 Presentation Time: 3:15pm-3:27pm
Presentation Time: 3:15pm-3:27pm
Location: Virtual
*Purpose: Belatacept (BELA) used for maintenance immunosuppression (IS) after kidney transplant (KT) shows similar graft and patient survival, but improved allograft function, despite more rejection when compared to calcineurin inhibitor (CNI). We postulated combining BELA with lymphocyte-depleting induction IS would improve rejection rate and retain safety.
*Methods: In a clinical protocol, the transplant surgeon and nephrologist planned IS and gave total dose of antithymocyte globulin (ATG) based on immunologic risk and tolerance of ATG. Belatacept (BELA) or tacrolimus (TAC) for primary maintenance IS was combined with mycophenolate and steroids. In retrospective analysis of sequential KTs, we used logistic regression to model the primary outcome of 1-year graft and patient survival with eGFR ≥45 mL/min in persons receiving BELA vs TAC.
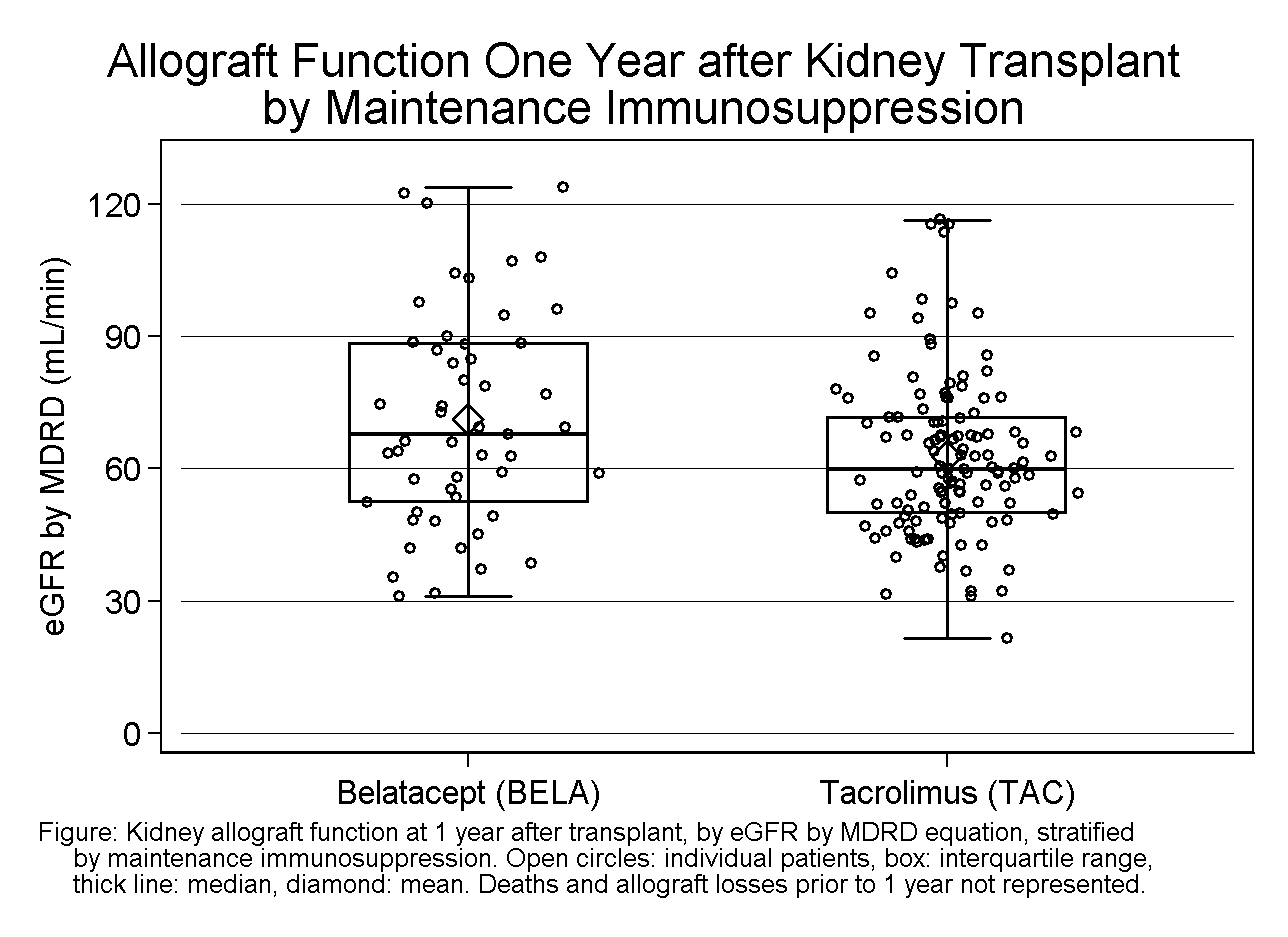
*Results: 181 KTs received either BELA (30%) or TAC (70%). Induction IS was basiliximab in 16 and ATG in 165 persons (101 had ATG >4.5 mg/kg and 64 had ATG ≤4.5 mg/kg). ATG was dose reduced in 51% vs 33% (p=0.03) and ESW by 30 days occurred in 5% vs 52% (p<0.001) of BELA vs TAC. Survival to 1 year with a functional allograft and eGFR ≥45 mL/min was 80% and 83% in BELA vs TAC, p=0.68. The mean eGFR at 1 year in functioning grafts was 71 mL/min with BELA and 63 mL/min with TAC, p=0.01 (Fig). Death, graft loss, rejection and infections were similar between groups (Table). PTLD developed in 1 person from each group, and Kaposi sarcoma occurred in 1 BELA patient. Controlling for age, sex, prior transplant, PRA, DSA, DGF, induction IS, and ESW, the odds ratio (OR) for the primary outcome was 0.74 (95%CI 0.24 - 2.3), p=0.61. A parsimonious model controlling for ATG >4.5mg/kg and ESW, the OR was 0.86 (95%CI 0.34 – 2.18), p=0.76 for BELA vs TAC.
*Conclusions: Belatacept-based maintenance IS was safe and effective when combined with ATG. Outcomes compared with CNI did not differ in terms of death, graft loss, rejection or infection events. Kidney function at 1 year was improved in the BELA group. Use of lymphocyte depleting induction IS may help reduce the higher rate of rejection in patients receiving BELA while maintaining comparable graft and patient survival.
| Outcome: | Belatacept (BELA), N=55: | Tacrolimus (TAC), N=126: | P-value: |
| Death, n (%): | 1 (2%) | 2 (2%) | 0.67 |
| Graft Loss, n (%): | 3 (5%) | 2 (2%) | 0.17 |
| eGFR<45 mL/min, n (%): | 7 (13%) | 18 (14%) | 0.48 |
| Rejection, n (%): | 13 (24%) | 28 (22%) | 0.83 |
| Serious Infection, n (%): | 26 (47%) | 60 (47%) | 0.97 |
| – CMV viremia, n (%): | 13 (24%) | 27 (21%) | 0.74 |
| – BK viremia, n (%): | 15 (27%) | 28 (22%) | 0.46 |
To cite this abstract in AMA style:
Goldman J, Mitrokhin A, Trivedi B, Vidyasagar V, Vadivel N, Goes N, Hart M. Belatacept versus Tacrolimus Combined with Antithymocyte Globulin in Kidney Transplantation [abstract]. Am J Transplant. 2020; 20 (suppl 3). https://atcmeetingabstracts.com/abstract/belatacept-versus-tacrolimus-combined-with-antithymocyte-globulin-in-kidney-transplantation/. Accessed May 26, 2026.« Back to 2020 American Transplant Congress