An Unexpected Case of Transthyretin Amyloid Cardiomyopathy (ATTR-CM) Overlooked Pretransplant, but Then Diagnosed Early After Kidney Transplant with a Negative Patient Outcome: A Case Report
W. Hoffman, M. Waybill, H. Yang, D. Ladie, M. Singh
UPMC Pinnacle Transplant, Harrisburg, PA
Meeting: 2021 American Transplant Congress
Abstract number: 899
Keywords: Heart failure, Kidney transplantation, Metabolic complications, Outcome
Topic: Clinical Science » Kidney » Kidney: Cardiovascular and Metabolic Complications
Session Information
Session Name: Kidney: Cardiovascular and Metabolic Complications
Session Type: Poster Abstract
Session Date & Time: None. Available on demand.
Location: Virtual
*Purpose: ATTR-CM is underrecognized and commonly overlooked and undiagnosed. When found it is often a late diagnosis in patients with severe left ventricular hypertrophy (LVH) and diastolic heart disease. These findings are common and non-specific in patients with end-stage renal disease (ESRD) making for a challenging diagnosis.
*Methods: We present a case of a 63-year-old female with a history significant for ESRD on hemodialysis, idiopathic chronic hypotension, and dysautonomia. She had a seemingly unremarkable pre-transplant workup including for the hypotension and then underwent a deceased donor kidney transplant admitted 4 weeks later with acute onset dyspnea.
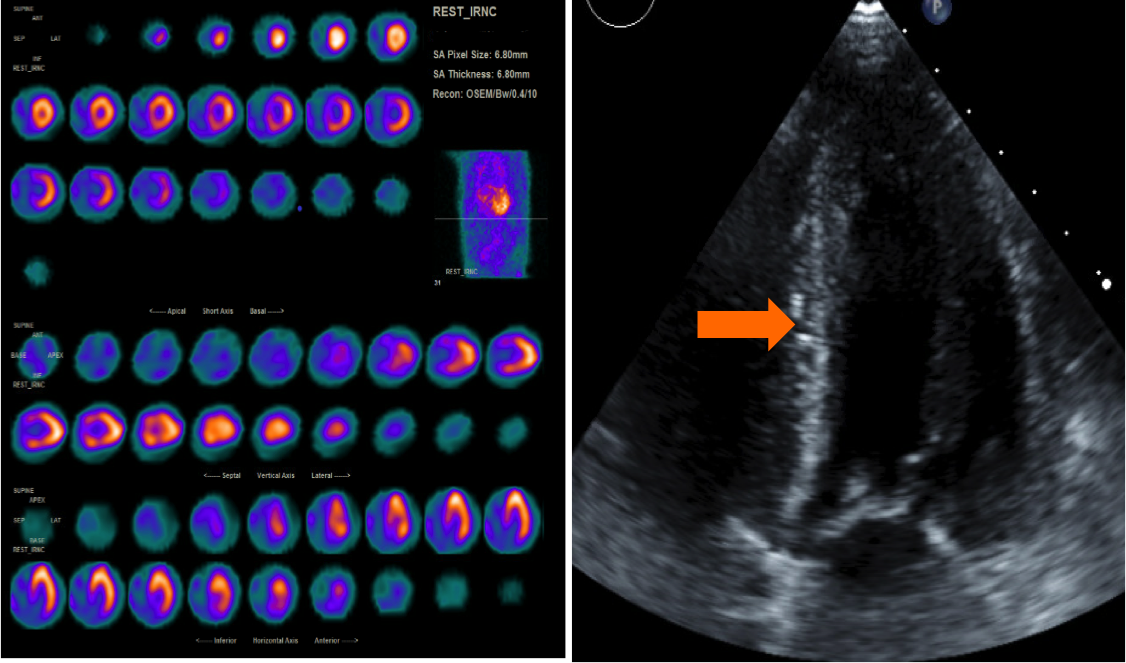
*Results: On that admission, the patient required renal replacement therapy for volume overload and acute kidney injury. A kidney transplant biopsy was consistent with acute tubular necrosis but was without acute rejection. Her Kidney function improved with a baseline creatinine of 1.8-2.2. A repeat echocardiogram found severe LVH with grade 2 diastolic dysfunction, unchanged from pre-transplant but now reported to have a speckled pattern suggestive of infiltrative cardiomyopathy. Congo red staining of the kidney biopsy was negative in the renal tissue but surprisingly positive in sampled extra-renal vascular tissue suggestive of systemic amyloidosis. Her clinical picture including the history of dysautonomia, EKG findings of low QRS voltage and AV block, and increased LV wall thickness were fitting of amyloidosis. The patient underwent a TcPYP (Technetium-pyrophosphate) scan that was highly suggestive of ATTR-CM. Serum and urine protein electrophoresis and immunofixation and serum-free light chain ratios were not consistent with an immunoglobulin light chain (AL) amyloidosis. Genetic testing for mutant ATTR (ATTRm) was also negative. The patient was therefore thought to likely have wild-type ATTR (ATTRwt) and was started on Tafamidis (transthyretin selective stabilizer) therapy. The patient was planned for an endomyocardial biopsy for a definitive diagnosis. Unfortunately, before this could be completed she succumbed to sudden death likely related to cardiac arrhythmia about 7 months post-transplant.
*Conclusions: This case demonstrates the need for high suspicion of cardiac amyloidosis in appropriate cases. The early and accurate diagnosis of ATTR cardiac amyloidosis is paramount given advances in noninvasive diagnostic modalities and treatment options.
To cite this abstract in AMA style:
Hoffman W, Waybill M, Yang H, Ladie D, Singh M. An Unexpected Case of Transthyretin Amyloid Cardiomyopathy (ATTR-CM) Overlooked Pretransplant, but Then Diagnosed Early After Kidney Transplant with a Negative Patient Outcome: A Case Report [abstract]. Am J Transplant. 2021; 21 (suppl 3). https://atcmeetingabstracts.com/abstract/an-unexpected-case-of-transthyretin-amyloid-cardiomyopathy-attr-cm-overlooked-pretransplant-but-then-diagnosed-early-after-kidney-transplant-with-a-negative-patient-outcome-a-case-report/. Accessed May 20, 2026.« Back to 2021 American Transplant Congress