Short Term Changes in HRQOL Following Kidney Transplantation.
JHU, Baltimore.
Meeting: 2016 American Transplant Congress
Abstract number: 155
Keywords: Kidney transplantation, Morbidity, Quality of life, Risk factors
Session Information
Session Name: Concurrent Session: Older and High Risk Kidney Transplant Recipients/Donors
Session Type: Concurrent Session
Date: Sunday, June 12, 2016
Session Time: 4:30pm-6:00pm
 Presentation Time: 4:54pm-5:06pm
Presentation Time: 4:54pm-5:06pm
Location: Ballroom A
Health-Related Quality of Life (HRQOL) is a patient-centered outcome that measures the impact of a disease and its treatment. This is particularly relevant to those with End Stage Renal Disease (ESRD) given the burden of this condition and its treatment (dialysis or kidney transplantation (KT)). Few studies describe the short-term changes in HRQOL in recipients after KT.
Methods: HRQOL was measured at KT and one month post-KT for 213 recipients enrolled in a cohort (6/2013-8/2015) at Johns Hopkins. Normalized summary physical component (PCS), mental component (MCS) and ESRD specific sub-scales were calculated on a 0-100 scale with higher scores indicating better HRQOL. Multinomial models were used to describe the change (better, worse or no change) in HRQOL accounting for age, gender, race, education and donor type.
Results: In this KT cohort with mean age of 53 yrs (SD=13) at KT, mean PCS was 41.6(SD=10.1), MCS was 53.5(SD=8.4) and the ESRD specific scores were 80.5(SD=14.0) for symptoms, 71.2(SD=21.3) for effects and 50.9(SD=28.8) for burden of kidney disease. One month post-KT, PCS scores had declined by 5.1 points(p<0.01), while MCS score had increased by 1.9 points(p=0.03) and ESRD specific scores had generally increased,(symptoms by 2.4, p=0.07; effects by 7.8, p<0.001; and, burden of ESRD scores by 17.3(p<0.01).11.3% of patients reported improvements in PCS, 24.4% improvements in MCS and 14.7%,25% and 25.9% improvement in HRQOL scores for symptom, effects and burden of ESRD. One month post-KT recipients with less education were more likely to experience change in MCS (worsened HRQOL RR: 4.49, 95%CI 1.37-14.74; improved HRQOL RR: 5.11, 95% CI 1.71-15.29). Females were more likely to experience improved MCS (RR: 3.09, 95%CI, 1.06-9.01) as well as a change in disease effect-related HRQOL (worsened HRQOL RR: 4.49, 95%CI 1.08-18.69; improved HRQOL RR: 3.09, 95% CI 1.16-8.24).
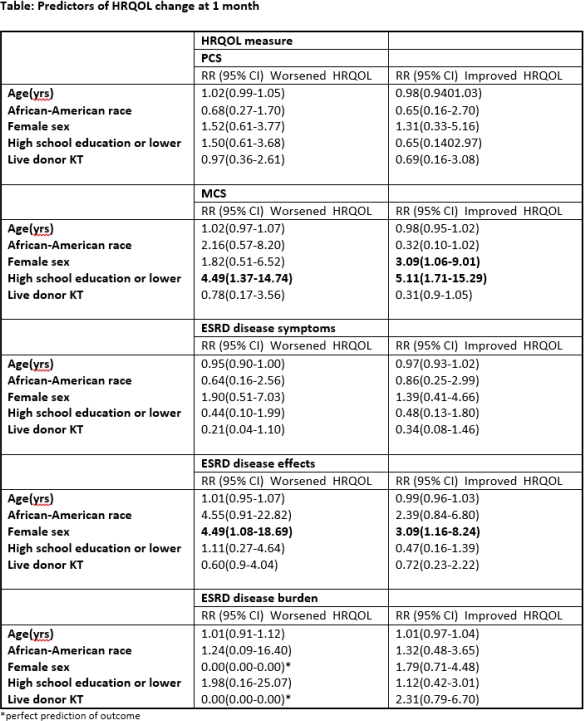
Conclusion: Physical HRQOL was worse one month after KT compared with at the time of KT; however, other subdomains of HRQOL showed improvement. Females and recipients without a college education had the greatest decline in HRQOL in one month after KT. Importantly, older recipients were not more likely to report worse HRQOL on any scale.
CITATION INFORMATION: Olorundare I, Ying H, McAdams-DeMarco M, Segev D. Short Term Changes in HRQOL Following Kidney Transplantation. Am J Transplant. 2016;16 (suppl 3).
To cite this abstract in AMA style:
Olorundare I, Ying H, McAdams-DeMarco M, Segev D. Short Term Changes in HRQOL Following Kidney Transplantation. [abstract]. Am J Transplant. 2016; 16 (suppl 3). https://atcmeetingabstracts.com/abstract/short-term-changes-in-hrqol-following-kidney-transplantation/. Accessed July 12, 2025.« Back to 2016 American Transplant Congress
