Non-Renal Factors Predicting Combined Liver-Kidney Transplantation for Non-Dialysis-Requiring Wait-Listed End Stage Liver Disease Patients: 14 Years of US Experience.
University of Florida, Gainesville, FL
Meeting: 2017 American Transplant Congress
Abstract number: 431
Keywords: Glomerular filtration rate (GFR), Kidney/liver transplantation, Liver transplantation
Session Information
Session Name: Concurrent Session: Kidney Issues in Liver Transplantation
Session Type: Concurrent Session
Date: Tuesday, May 2, 2017
Session Time: 2:30pm-4:00pm
 Presentation Time: 3:42pm-3:54pm
Presentation Time: 3:42pm-3:54pm
Location: E451b
OBJECTIVE: We aimed to identify the non-renal factors associated with the higher likelihood of combined liver-kidney transplantation (CLKT) vs. liver transplantation alone (LTA) in end stage liver disease (ESLD) patients not requiring dialysis (NOD) or qualified for preemptive kidney transplant alone at the time of wait-listing for liver transplant.
PATIENTS AND METHODS: Based on OPTN data as of March 31,2016, we studied adult ESLD patients wait-listed for liver transplant in July 2002-March 2016 with modification of diet in renal disease (MDRD) equation-estimated glomerular filtration rate (GFR) of >20 ml/min and NOD. The outcome of the study was CLKT or LTA. Patients who had not received a CLKT or LTA after wait-listing, died on the wait-list, received other (except renal) organ or a living donor liver transplant, or received dialysis in the wk. before CLKT or LTA were excluded from the analysis. We used logistic regression analysis to determine odds ratio and 95% confidence interval for CLKT vs. LTA associated with risk factors.
RESULTS: Out of 31,072 liver transplant candidates, MDRD- GFR was >30 ml/min. in 28,988 (93.3%) and <30 ml/min. in 2084 (6.7%) at LT wait-listing. At the time of CLKT or LTA, MDRD-GFR was >30 ml/min in 26,152 (84.2%) and <30 ml/min in 4,897 (15.8%) patients: CLKT rates were 1.38% (n=361) and 16.8% (n=823); respectively.
The strongest predictors of CLKT vs. LAT were: MDRD-GFR at both wait-listing and transplant and MELD score at transplant. In decreasing point estimates, the non-renal risk factors for CLKT vs. LTA were: wait-list duration; previous liver transplant; recipient history of diabetes, African American ethnicity, age >65 yr., need for life support, Hispanic ethnicity and age 50-64 yr.; and transplant era, 2009-2016. The likelihood of CLKT vs. LTA was lower with: donor age and liver transplant volume in the hospital-venue of CLKT or LAT (Figure 1).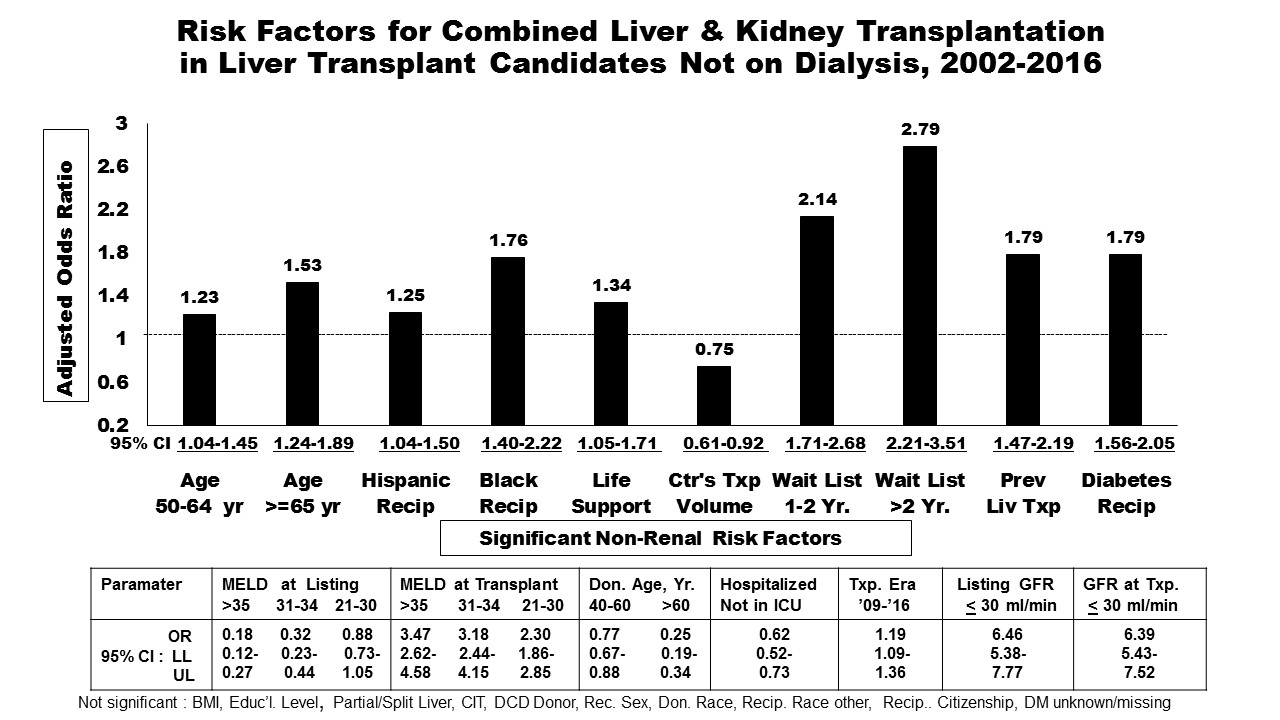 CONCLUSION: Aside from MELD score and MDRD-GFR, there are significant non-renal risk factors associated with higher likelihood of CLKT vs. LTA in non-dialysis-requiring liver transplant candidates.
CONCLUSION: Aside from MELD score and MDRD-GFR, there are significant non-renal risk factors associated with higher likelihood of CLKT vs. LTA in non-dialysis-requiring liver transplant candidates.
CITATION INFORMATION: Santos A, Casey M, Alquadan K, Gregg J, Womer K. Non-Renal Factors Predicting Combined Liver-Kidney Transplantation for Non-Dialysis-Requiring Wait-Listed End Stage Liver Disease Patients: 14 Years of US Experience. Am J Transplant. 2017;17 (suppl 3).
To cite this abstract in AMA style:
Santos A, Casey M, Alquadan K, Gregg J, Womer K. Non-Renal Factors Predicting Combined Liver-Kidney Transplantation for Non-Dialysis-Requiring Wait-Listed End Stage Liver Disease Patients: 14 Years of US Experience. [abstract]. Am J Transplant. 2017; 17 (suppl 3). https://atcmeetingabstracts.com/abstract/non-renal-factors-predicting-combined-liver-kidney-transplantation-for-non-dialysis-requiring-wait-listed-end-stage-liver-disease-patients-14-years-of-us-experience/. Accessed April 19, 2024.« Back to 2017 American Transplant Congress
